Botox Injections for Gastroparesis: A New Approach to Stomach Motility
A novel endoscopic method may ease chronic gastric pain by relaxing the stomach outlet.
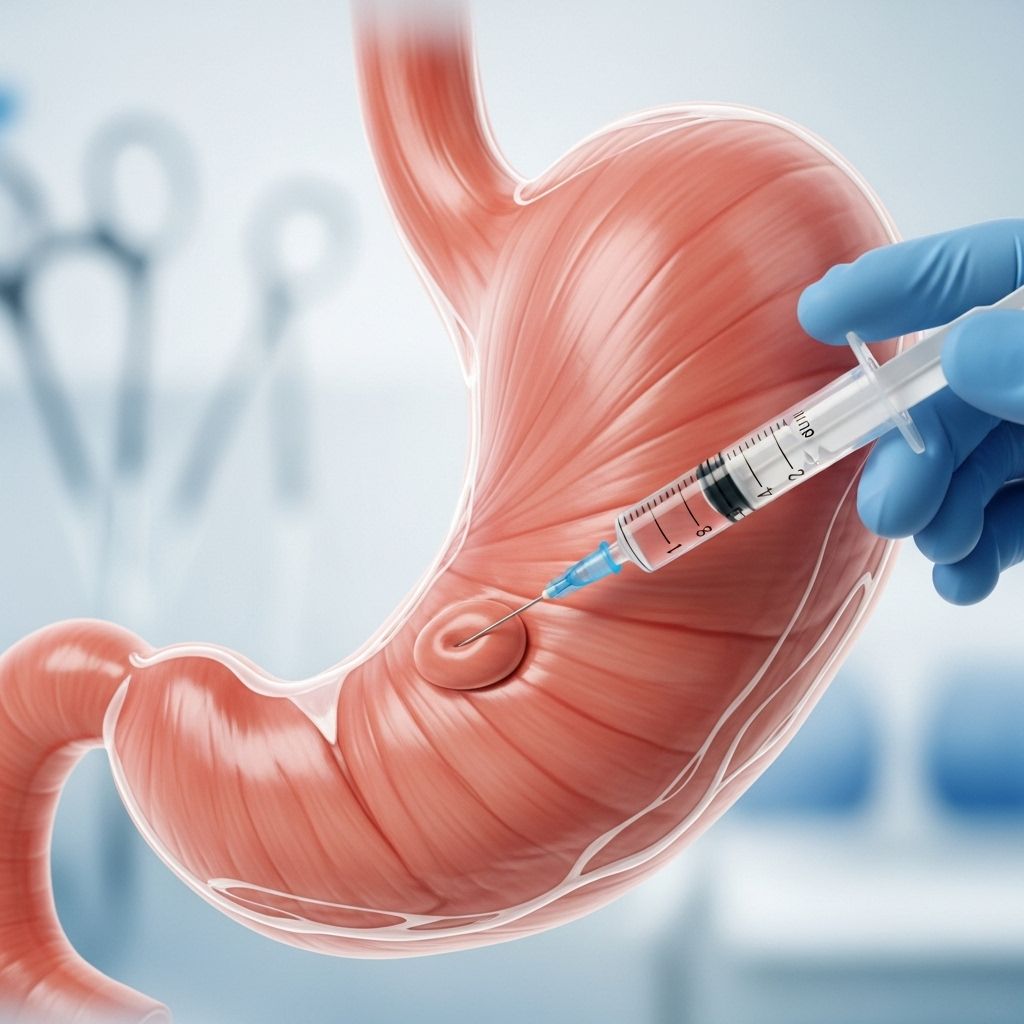
Gastroparesis is a chronic digestive disorder that disrupts how the stomach empties food, leading to symptoms such as persistent nausea, vomiting, bloating, weight loss, and abdominal discomfort. Treating this condition has proven especially challenging when standard medications and diet changes fail. A new approach—injecting Botox directly into the stomach—offers hope for patients seeking improved quality of life and relief from daily symptoms.
What Is Gastroparesis?
Gastroparesis is a long-term motility disorder where the stomach cannot empty food effectively, causing food to move through the digestive tract much more slowly than normal. Damage to the stomach’s nerves, especially the vagus nerve, is thought to be a root cause. Common symptoms include:
- Nausea and vomiting
- Loss of appetite
- Weight loss
- Bloating
- Heartburn
- Upper abdominal pain
This disorder is often seen in people with diabetes, but it can also occur for unknown reasons (idiopathic gastroparesis) or after surgery.
Traditional Treatments for Gastroparesis
Historically, treatment options have centered on dietary modifications and medications that help improve stomach emptying. Common interventions include:
- Eating small, frequent meals
- Avoiding high-fat and high-fiber foods
- Taking prokinetic drugs (e.g., metoclopramide, domperidone) to stimulate stomach contractions
- Antiemetic medications for nausea
- Other drugs like erythromycin or cisapride (though each has limitations and possible side effects)
Despite these treatments, many patients experience little improvement, prompting the search for new therapeutic strategies.
How Botox Treats Gastroparesis
Botulinum toxin type A—commonly known as Botox—is widely recognized as a muscle relaxant for cosmetic and medical uses. In the treatment of gastroparesis, Botox is injected via endoscopy directly into the pylorus, the muscular valve between the stomach and the small intestine. The main objective: Relax the pylorus to allow food to pass more easily from the stomach into the intestines.
| Traditional Therapy | Botox Injection Therapy |
|---|---|
| Focuses on whole digestive tract | Targets specific stomach muscle (pylorus) |
| Potential for systemic side effects | Minimizes systemic impact |
| May offer limited symptom relief | Can dramatically reduce key symptoms temporarily |
Injection Procedure and Mechanism
The procedure is performed via an endoscope, inserted through the mouth and into the stomach, allowing physicians to inject Botox into the pyloric sphincter muscle. The toxin works by blocking the release of acetylcholine, a neurotransmitter responsible for muscle contractions, leading to temporary muscle relaxation. As a result, the pyloric valve stays open longer, improving gastric emptying and reducing symptoms.
- Typically requires sedation, but not general anesthesia
- Outpatient procedure—patients often return home the same day
- Benefits usually last a few months; repeat injections may be necessary
Patient Experiences: New Hope for Symptom Relief
Clinical experience and ongoing studies have revealed a spectrum of outcomes for patients who undergo Botox injection therapy for gastroparesis.
In a retrospective analysis cited by experts, roughly 72% of treated patients reported significant symptom improvement (over 50% reduction in severity). Notably, men and those with idiopathic gastroparesis seemed to benefit most. Furthermore, 24% reported fewer emergency room visits or hospitalizations following treatment. Among non-responders, some progressed to surgical options like gastric electrical stimulation.
Other studies focused on diabetic gastroparesis have echoed these improvements: Patients experienced notable reductions in nausea, vomiting, and early satiety, and even achieved weight gain after chronic episodes of weight loss and appetite loss. Minimal complications are reported, and the approach is generally considered safe when performed by skilled gastroenterologists.
Limitations and Need for Repeat Procedures
It is important to note that the effects of injected Botox are temporary. Most individuals see benefits for weeks or months before symptoms gradually return, necessitating additional injections. Moreover, while patient-reported improvements are significant, randomized controlled trials have yielded mixed results, with some studies showing no superiority over placebo saline injections. This has led some medical societies to refrain from recommending routine Botox therapy for all gastroparesis patients.
Potential Risks and Drawbacks
- Effectiveness and duration vary widely among individuals
- May complicate future stomach surgery if needed
- Temporary solution—does not cure the underlying disorder
- Risk of infection or bleeding (though rare with skilled providers)
Who Is a Candidate for Botox Therapy?
Patients struggling with refractory gastroparesis—those who have failed dietary and pharmacologic interventions—may be considered for Botox treatment. Physicians assess each patient’s case, considering disease cause (diabetic, idiopathic, or postsurgical), overall health, and prior treatment outcomes. Repeat injections are sometimes necessary, and individuals with more severe delayed gastric emptying may require additional treatments or procedures.
Expert Perspectives and Research
The scientific community has not reached consensus regarding Botox injection’s place in gastroparesis management. Open-label trials and patient surveys consistently report symptom improvements, while randomized controlled trials remain less encouraging, failing to show consistent superiority versus placebo in diverse patient populations.
A summary of evidence:
- Open-label studies: Most patients experience relief and improvements in quality of life.
- Randomized trials: Mixed results—some fail to show statistical difference over placebo.
- Retrospective analyses: Positive results in subgroups, especially men and those with idiopathic gastroparesis.
Given the limited available drug therapies and failure of medical management in many cases, clinicians continue to explore and refine the use of Botox as a potential tool for those with severe, persistent symptoms.
What Do Gastroenterologists Say?
Leading experts recommend an individualized approach. For patients who have exhausted dietary and medicinal options, and before progressing to surgical procedures, Botox injections at the pylorus may offer valuable symptom relief without substantial systemic side effects.
Living With Gastroparesis: Managing Day-to-Day Life
Gastroparesis can have profound effects on an individual’s physical and emotional well-being. While Botox therapy represents one option, comprehensive management also includes:
- Close collaboration with healthcare professionals (gastroenterologists, dietitians)
- Customized nutrition plans (e.g., blended foods, liquid diets)
- Education about portion control and avoidance of trigger foods
- Stress management strategies to support quality of life
Patients and their families are encouraged to stay proactive and open-minded as new therapies continue to emerge.
Frequently Asked Questions (FAQs)
How do Botox injections help with gastroparesis?
Botox injections relax the pyloric valve muscle at the outlet of the stomach, allowing food to move through to the small intestine more efficiently, which can reduce nausea, vomiting, and abdominal discomfort.
Are Botox injections a permanent cure for gastroparesis?
No, Botox injections offer temporary relief. Effects may last from a few weeks to several months, after which symptoms may return and repeat treatment could be necessary.
What are the risks of Botox injections for gastroparesis?
Risks are generally low when performed by an experienced gastroenterologist but can include infection, bleeding, minor discomfort or reflux. Botox injections might also make future stomach surgery more challenging if it becomes necessary.
Do all patients with gastroparesis benefit from Botox injections?
Outcomes vary. While many patients report significant symptom improvement, others see little or no change. Randomized trials have not consistently shown benefits over placebo in all cases.
Is the procedure painful? Will I need anesthesia?
Most patients receive sedation during the procedure to minimize discomfort. It is typically done as an outpatient and is not considered highly painful.
Can Botox injections affect other parts of my body?
The procedure is targeted to the stomach’s pyloric muscle, minimizing widespread or systemic effects that are more common with oral medications.
How is gastroparesis diagnosed?
Diagnosis involves symptom review, physical examination, imaging studies (such as solid phase gastric emptying tests), and exclusion of mechanical obstructions.
What happens if Botox injections do not work for me?
Patients who do not respond to Botox may be considered for alternative therapies, such as gastric electrical stimulation or surgical interventions. Continued dialogue with healthcare providers is key for exploring all available options.
Key Takeaways
- Botox injections into the pylorus can offer significant but temporary symptom relief for many gastroparesis patients who have failed conventional therapies.
- The procedure is generally safe and well-tolerated, requiring only sedation and an outpatient visit.
- Results vary, with some patients experiencing marked improvement and others finding little benefit, underlining the importance of individualized care.
- Gastroparesis management is complex and should incorporate dietary strategies, medical therapies, and procedural innovations like Botox injections under specialist guidance.
Further Reading & Resources
- Consult your gastroenterologist for an assessment tailored to your specific needs.
- Local and national gastroparesis advocacy groups can offer support and education.
- Ongoing clinical trials may provide access to innovative therapies for eligible patients.
References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4501969/
- https://www.wsh.nhs.uk/CMS-Documents/Patient-leaflets/Endoscopy/6542-1-Gastroscopy-with-injection-of-Clostridium-botulinim-Botox-for-the-treatment-of-achalasia-and-Gastroparesis.pdf
- https://diabetesjournals.org/care/article/27/10/2341/23226/The-Treatment-of-Diabetic-Gastroparesis-With
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6223662/
- https://pure.johnshopkins.edu/en/publications/botulinum-toxin-injection-for-treatment-of-gastroparesis
- https://digitalcommons.pcom.edu/cgi/viewcontent.cgi?article=1192&context=pa_systematic_reviews
- https://davidyaminimd.com/gastroparesis-treatments/
Read full bio of medha deb












