Ulcerative Colitis: Symptoms, Causes, Risk Factors, and Types
Gain a thorough understanding of ulcerative colitis—its symptoms, causes, affected groups, and complications.
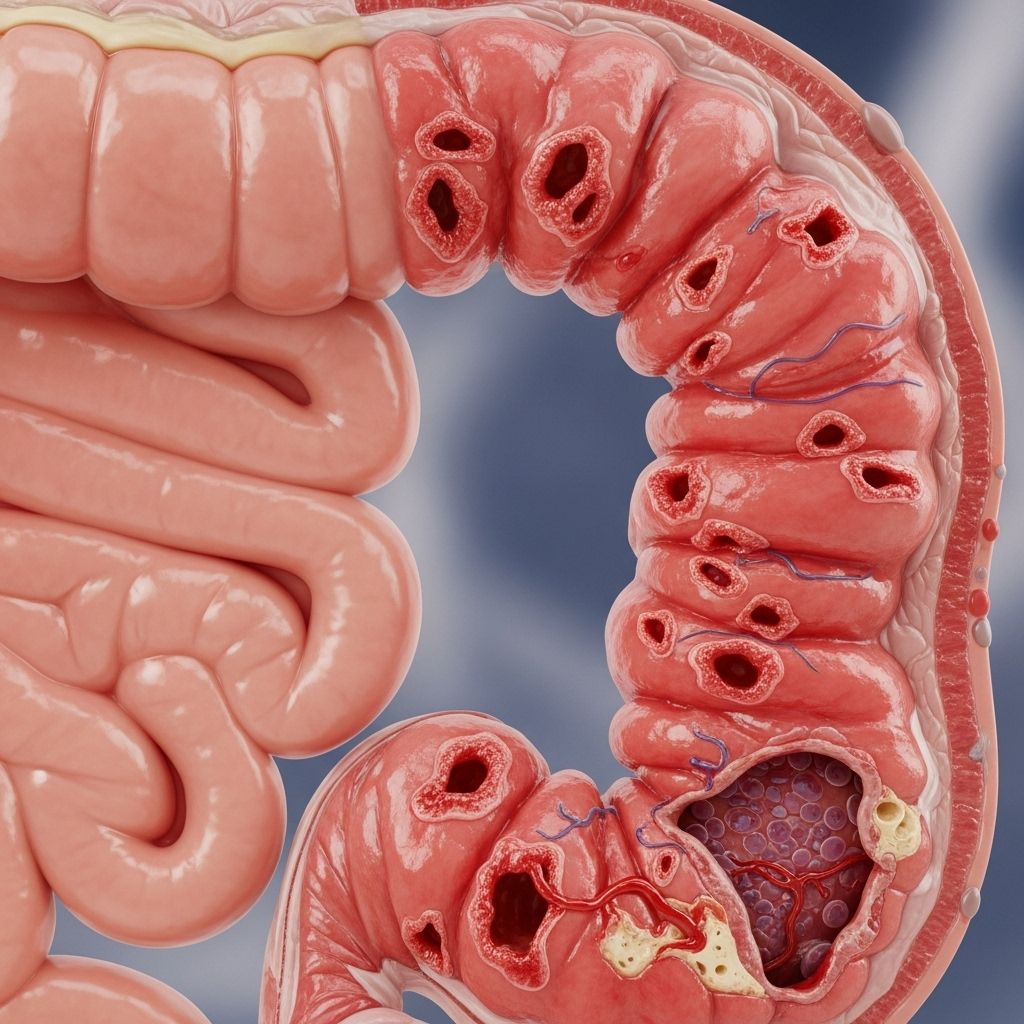
Ulcerative colitis is a chronic inflammatory disease that affects the lining of the large intestine (colon) and rectum. The disease causes inflammation and ulcers in the digestive tract, which can lead to a variety of symptoms that may develop over time. While the exact cause remains uncertain, several factors, including the immune response and genetics, have been identified as potential contributors. This article offers a comprehensive examination of ulcerative colitis, covering its symptoms, types, causes, risk factors, complications, and when it is important to seek medical attention.
What Is Ulcerative Colitis?
Ulcerative colitis is categorized as an inflammatory bowel disease (IBD). It primarily strikes the innermost lining of the colon and rectum, resulting in ongoing inflammation, ulceration, and sometimes severe digestive disruption. The disease often manifests with periods of exacerbation (flare-ups) and remission (fewer or no symptoms).
Who Gets Ulcerative Colitis?
The onset of ulcerative colitis can occur at any stage of life, but it is most commonly diagnosed in individuals before the age of 30. That said, it can also begin later, with some people developing the disease after age 60. Both men and women are affected at similar rates.
There are several factors that increase the likelihood of developing ulcerative colitis:
- Family history: Having a first-degree relative (such as a parent, sibling, or child) with ulcerative colitis raises the risk of developing the condition.
- Ethnicity: White individuals are at highest risk. Among whites, people of Ashkenazi Jewish descent show especially high prevalence.
- Genetics: Certain genetic markers have been associated with the disease.
While diet and stress do not cause ulcerative colitis, they can trigger or aggravate symptoms and flare-ups.
Symptoms of Ulcerative Colitis
Symptoms of ulcerative colitis can vary widely, primarily depending on the severity of the inflammation and the specific area of the colon affected. Approximately half of those with ulcerative colitis experience mild to moderate symptoms, but for some, symptoms can become severe. The disease may be punctuated by remission, where symptoms improve or disappear for a time, before returning in flare-ups.
Common Symptoms
- Diarrhea, often containing blood or pus.
- Rectal bleeding, sometimes visible when passing stools.
- Abdominal pain and cramping.
- Rectal pain.
- Urgency to pass stool.
- Inability to pass stool despite urgency (tenesmus).
- Unintended weight loss.
- Fatigue.
- Fever.
- Children may experience delayed or impaired growth and development.
When to See a Doctor
If you notice a persistent change in your bowel habits or experience symptoms that may suggest ulcerative colitis, consult a healthcare professional, especially if you have:
- Ongoing abdominal pain
- Blood in your stool
- Diarrhea that does not improve with over-the-counter treatments
- Diarrhea severe enough to wake you at night
- An unexplained fever lasting longer than one to two days
While ulcerative colitis is rarely fatal, complications can be life-threatening in some cases and medical guidance is crucial.
Types of Ulcerative Colitis
Doctors classify ulcerative colitis into different types based on which parts of the colon and rectum are involved. The main types include:
- Ulcerative proctitis: Inflammation is limited to the rectum, the area nearest the anus. Often, rectal bleeding and difficulty with bowel movements are the primary symptoms.
- Left-sided colitis: Inflammation extends from the rectum through the sigmoid and descending colon. This includes proctosigmoiditis, which involves both the rectum and sigmoid colon. Symptoms may involve bloody diarrhea, abdominal cramps and pain, and tenesmus (urgency without the ability to pass stool).
- Extensive (pancolitis): Widespread inflammation affects the entire colon. This more severe form can cause intense and persistent bloody diarrhea, abdominal cramps, fatigue, and notable weight loss.
Causes of Ulcerative Colitis
The exact cause of ulcerative colitis remains unknown; however, several factors are thought to contribute to its development.
- Immune system abnormalities: A frequently cited hypothesis is an abnormal immune response. In ulcerative colitis, the immune system mistakenly attacks the cells of the digestive tract when defending against invading organisms (such as viruses or bacteria).
- Genetic inheritance: Multiple genetic markers have been associated with ulcerative colitis. People who have family members with the condition are more likely to develop the disease.
- Environmental triggers: While not direct causes, certain environmental factors such as infections may initiate or exacerbate the disease in predisposed individuals.
Older beliefs linked diet and stress as direct causes, but the current consensus is that they only worsen symptoms in susceptible people rather than cause the disease itself.
Risk Factors
The following factors can heighten the risk of developing ulcerative colitis:
- Age: Most individuals are diagnosed before 30 years old, but it can occur at any age, including after age 60.
- Ethnicity: People of white ethnicity, especially those of Ashkenazi Jewish descent, have the greatest risk, although all races can develop the disease.
- Family history: Having a close relative with ulcerative colitis greatly increases risk.
Men and women are equally susceptible to developing ulcerative colitis.
Complications of Ulcerative Colitis
Over time, untreated or severe ulcerative colitis may result in significant complications, some of which are potentially serious or life-threatening. These can include:
- Severe dehydration: Extensive diarrhea may result in dehydration requiring immediate intervention.
- Perforated colon: Chronic inflammation can weaken and eventually cause rupture of the colon wall.
- Chronic anemia: Ongoing bleeding and poor nutrient absorption can produce persistent anemia.
- Bone loss: Reduced bone density (osteoporosis) can occur due to both the disease and certain medications used in its treatment.
- Increased risk of blood clots: People with ulcerative colitis are more prone to developing clotting in veins and arteries.
- Colon cancer: The risk of colon cancer rises the longer the disease is present, particularly if the entire colon is affected.
- Inflammation in other organs: Ulcerative colitis can trigger swelling and discomfort in the skin, joints, and eyes.
- Growth delays in children: Ongoing inflammation can impair physical development in pediatric patients.
Summary Table: Ulcerative Colitis at a Glance
| Aspect | Description |
|---|---|
| Most Common Age of Onset | Before 30 years, but possible at any age |
| Major Symptoms | Bloody diarrhea, abdominal pain, rectal bleeding, bowel urgency, fatigue, weight loss |
| Types | Ulcerative proctitis, left-sided colitis, extensive (pancolitis) |
| Risk Groups | Those with family history, white ethnicity (notably Ashkenazi Jewish background) |
| Primary Complications | Dehydration, perforated colon, anemia, bone loss, blood clots, colon cancer, extraintestinal inflammation |
| Cause | Unknown; relates to immune dysfunction and genetics |
Frequently Asked Questions (FAQs)
Q: What is the difference between ulcerative colitis and Crohn’s disease?
A: Both are types of inflammatory bowel disease, but ulcerative colitis affects only the colon and rectum’s lining, while Crohn’s disease can impact any part of the digestive tract and may penetrate deeper bowel layers.
Q: Is ulcerative colitis a lifelong condition?
A: Yes, ulcerative colitis is chronic. While it may have extended periods of remission, it does not currently have a cure. Management focuses on symptom control and prevention of complications.
Q: Can changes in diet cure ulcerative colitis?
A: No, dietary changes cannot cure ulcerative colitis, though certain foods may worsen or relieve symptoms. Consultation with a healthcare provider or nutritionist is advised for personalized dietary guidance.
Q: What triggers flare-ups of ulcerative colitis?
A: Flare-ups may be triggered by stress, certain foods, infections, or missing medication. However, the exact triggers can vary among individuals.
Q: Does ulcerative colitis increase the risk of colon cancer?
A: Yes, having ulcerative colitis, especially for many years or with extensive colon involvement, raises the risk of colon cancer. Regular colonoscopic screening is recommended for those with the disease.
Resources & Support
If you or someone you know is struggling with ulcerative colitis, consult a gastroenterologist for diagnosis and management. Support groups and educational resources are also available through organizations such as the Crohn’s & Colitis Foundation.
References
- https://www.mayoclinic.org/diseases-conditions/ulcerative-colitis/symptoms-causes/syc-20353326
- https://www.mayoclinic.org/diseases-conditions/inflammatory-bowel-disease/symptoms-causes/syc-20353315
- https://www.youtube.com/watch?v=z_ddz4WAY18
- https://www.mayoclinic.org/diseases-conditions/ulcerative-colitis/diagnosis-treatment/drc-20353331
- https://newsnetwork.mayoclinic.org/discussion/signs-and-symptoms-of-ulcerative-colitis/
- https://www.mayoclinic.org/diseases-conditions/microscopic-colitis/symptoms-causes/syc-20351478
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/living-with-crohns-disease-or-colitis
- https://www.mayoclinic.org/diseases-conditions/ulcerative-colitis/in-depth/ulcerative-colitis-flare-up/art-20120410
- https://www.youtube.com/watch?v=2JXL3_IRBdc
Read full bio of medha deb