Rectal Bleeding: Causes and When to Seek Care
Uncover the most common and rare causes of rectal bleeding and learn when to seek prompt medical attention.
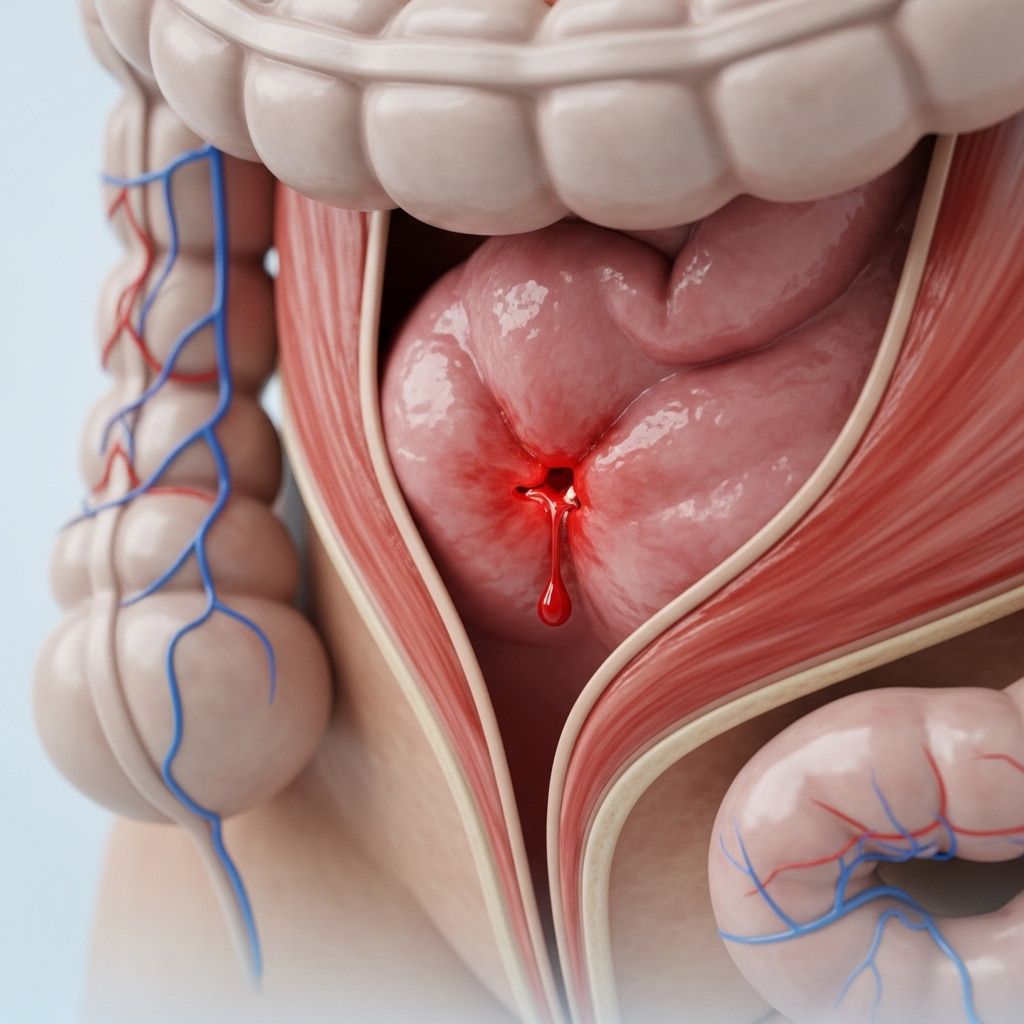
Rectal bleeding refers to any blood that passes from the anus, often noticed as blood in your stool, on toilet paper, or in the toilet bowl. The color can range from bright red to dark maroon, depending on the bleeding site. Understanding the underlying causes of rectal bleeding is important for knowing when to seek medical attention. This article details the common and less common causes of rectal bleeding, along with guidance on when to consult a healthcare professional.
What is Rectal Bleeding?
Rectal bleeding typically describes blood passing from the anus, often associated with bleeding from the lower colon or rectum. Symptoms can include:
- Bright red blood on toilet paper or in the toilet bowl
- Streaks of blood on stool
- Sometimes, darker or maroon colored blood mixed in stool
The amount can vary from a small spot to heavy bleeding. Even minimal blood loss warrants evaluation, especially with other symptoms.
Common Causes of Rectal Bleeding
Several conditions cause rectal bleeding; the following are the most frequent:
- Anal fissure – A small tear in the lining of the anal canal, often caused by passing hard or large stools, can lead to pain and bleeding.
- Constipation – Chronic constipation increases the risk of straining, contributing to fissures and hemorrhoids.
- Hard stools – Passing firm or dry stools can injure the anus or rectal lining, leading to small bleeds.
- Hemorrhoids – Swollen, inflamed veins in the anus or rectum are a leading source of rectal bleeding, often resulting in bright red blood that may coat stool or appear on toilet paper.
Less Common Causes of Rectal Bleeding
Beyond the typical culprits, many less common conditions can also result in rectal bleeding:
- Anal cancer – A rare cancer that can cause visible bleeding, discomfort, or even a lump near the anus.
- Angiodysplasia – Abnormal blood vessel formation in the intestines, which can cause intermittent and sometimes heavy bleeding.
- Colon cancer – Malignant growths in the colon may bleed and often manifest with other symptoms such as changes in bowel habits or weight loss.
- Colon polyps – Benign or precancerous growths on the colon lining can cause mild, painless bleeding, especially as they enlarge.
- Crohn’s disease – This inflammatory bowel disease causes inflammation and sometimes ulceration of the digestive tract, leading to bleeding.
- Diarrhea – Frequent loose stools can irritate the rectal lining and sometimes cause bleeding.
- Diverticulosis – Small bulges in the intestine wall (diverticula) may occasionally bleed, causing sudden painless rectal bleeding.
- Inflammatory bowel disease (IBD) – A group of disorders including Crohn’s disease and ulcerative colitis that involve chronic inflammation and can cause rectal bleeding.
- Ischemic colitis – Reduction in blood flow to the colon triggers inflammation and sometimes bleeding.
- Proctitis – Inflammation of the rectal lining, often resulting in discomfort and bleeding.
- Pseudomembranous colitis – Inflammation of the colon due to certain infections (e.g., Clostridioides difficile), which can cause bleeding.
- Radiation therapy – Post-radiation changes in rectal tissues may lead to chronic or recurrent bleeding.
- Rectal cancer – Cancer in the lower intestine may bleed slowly (often unnoticed) or cause more obvious bleeding.
- Solitary rectal ulcer syndrome – A rare disorder involving ulceration of the rectal lining, presenting as bleeding and sometimes a sense of incomplete evacuation.
- Ulcerative colitis – Chronic inflammation of the colon lining produces ulcers, often resulting in rectal bleeding.
Detailed Overview of Key Causes
| Cause | Description | Typical Symptoms |
|---|---|---|
| Hemorrhoids | Swollen veins in rectum/anus | Bright red blood, itching, pain (external hemorrhoids) |
| Anal fissure | Small tear in anal lining | Pain with bowel movements, blood on toilet paper |
| Diverticulosis | Pouches in colon wall that may bleed | Painless, sudden bleeding |
| Colon cancer/polyps | Benign or malignant growths | Rectal bleeding, change in stool, unexplained weight loss |
| Inflammatory Bowel Disease (IBD) | Chronic colon inflammation (includes Crohn’s, ulcerative colitis) | Abdominal pain, diarrhea, bleeding |
| Proctitis | Rectal inflammation | Pain, bleeding, feeling of incomplete evacuation |
Other Contributing Factors
- Straining during bowel movements increases the likelihood of fissures and hemorrhoids.
- Chronic diarrhea or persistent constipation can irritate rectal tissues, leading to bleeding.
- Radiation or chemotherapy can make rectal tissues more fragile and prone to bleeding episodes.
How Rectal Bleeding May Appear
The nature and appearance of rectal bleeding often provides clues about the underlying cause:
- Bright red blood on toilet paper or in the bowl: Usually signals bleeding low in the colon, rectum, or anus—commonly from hemorrhoids or fissures.
- Blood mixed with stool: May indicate bleeding higher up in the colon or rectum, such as from colon polyps, cancer, or IBD.
- Dark or maroon blood: Sometimes results from higher (proximal) colon sources or more rapid intestinal transit.
When to Seek Medical Care
Rectal bleeding is seldom an emergency, but prompt medical assessment is important, especially in the presence of risk factors or worrisome signs. You should seek immediate medical help if there is significant or persistent rectal bleeding, or if any of the following occur:
- Dizziness or fainting
- Rapid heartbeat
- Shortness of breath
- Severe abdominal pain
- Bleeding that does not stop or is rapidly worsening
Schedule an appointment with your healthcare provider if you experience:
- Rectal bleeding lasting more than two days
- Blood appears repeatedly in stools
- Bleeding accompanied by unexplained weight loss, change in stool habits, or persistent abdominal discomfort
- Any concerns about new or unexplained rectal bleeding
Diagnosis and Evaluation
To determine the cause of rectal bleeding, your doctor may:
- Take a medical history and perform a physical examination
- Recommend a rectal exam or anoscopy to directly visualize the anal canal
- Order blood tests to check for anemia or infection
- Request diagnostic imaging (CT scans, barium enema, or MRI in some cases)
- Recommend colonoscopy or sigmoidoscopy for a detailed view of the colon and rectum, and to take biopsies if necessary
Prevention and Self-care Tips
- Eat a high-fiber diet to soften stool and reduce straining
- Drink adequate fluids, especially water
- Exercise regularly to support healthy bowel function
- Avoid prolonged sitting on the toilet or excessive straining
- Promptly treat constipation and diarrhea
Frequently Asked Questions (FAQs)
Q: Is rectal bleeding always a sign of cancer?
No. While cancer can cause rectal bleeding, most cases are due to benign conditions like hemorrhoids or fissures. However, persistent or unexplained bleeding should always be checked by a doctor.
Q: What color is the blood in rectal bleeding?
Typically, blood from lower sources (rectum or anus) appears bright red, while bleeding further up the colon may look dark red or maroon.
Q: Should I be concerned if bleeding is a one-time event?
Minor bleeding from a one-time episode, especially with hard stools, may not be serious. However, recurrent bleeding or any associated symptoms—like pain, weight loss, or reduced appetite—should be evaluated.
Q: Can hemorrhoids go away on their own?
Mild hemorrhoids may resolve with lifestyle changes such as increased fiber intake and hydration. Persistent or painful hemorrhoids may require medical treatment.
Q: What are the emergency symptoms related to rectal bleeding?
Seek emergency care if you have heavy bleeding, dizziness, rapid heartbeat, fainting, or severe abdominal pain.
Summary Table: Most and Least Common Causes
| Most Common Causes | Less Common Causes |
|---|---|
|
|
Conclusion
Rectal bleeding has many possible causes, ranging from minor irritation to serious medical conditions like colorectal cancer. It is always wise to discuss any rectal bleeding with your doctor to identify the underlying cause and ensure appropriate care. Early evaluation is especially important if you have additional symptoms or risk factors. Proactive attention to bowel health and routine screening helps reduce the risk of serious complications associated with rectal bleeding.
References
- https://www.mayoclinic.org/symptoms/rectal-bleeding/basics/causes/sym-20050740
- https://www.mayoclinic.org/diseases-conditions/proctitis/symptoms-causes/syc-20376933
- https://www.mayoclinic.org/diseases-conditions/gastrointestinal-bleeding/symptoms-causes/syc-20372729
- https://my.clevelandclinic.org/health/symptoms/14612-rectal-bleeding
- https://www.kuh.ku.edu.tr/mayo-clinic-care-network/mayo-clinic-health-information-library/symptoms/rectal-bleeding
- https://www.mayoclinic.org/symptom-checker/blood-in-stool-in-adults-adult/related-factors/itt-20009075
- https://www.mayoclinic.org/symptoms/rectal-bleeding/in-depth/definition/sym-20050740
- https://www.mayoclinic.org/diseases-conditions/hemorrhoids/symptoms-causes/syc-20360268
- https://www.amerikanhastanesi.org/mayo-clinic-care-network/mayo-clinic-health-information-library/symptoms/rectal-bleeding
Read full bio of Sneha Tete