Plantar Warts: Symptoms, Causes, Diagnosis, and Prevention
A comprehensive guide to understanding plantar warts: symptoms, causes, risk factors, when to see a doctor, and strategies for prevention.
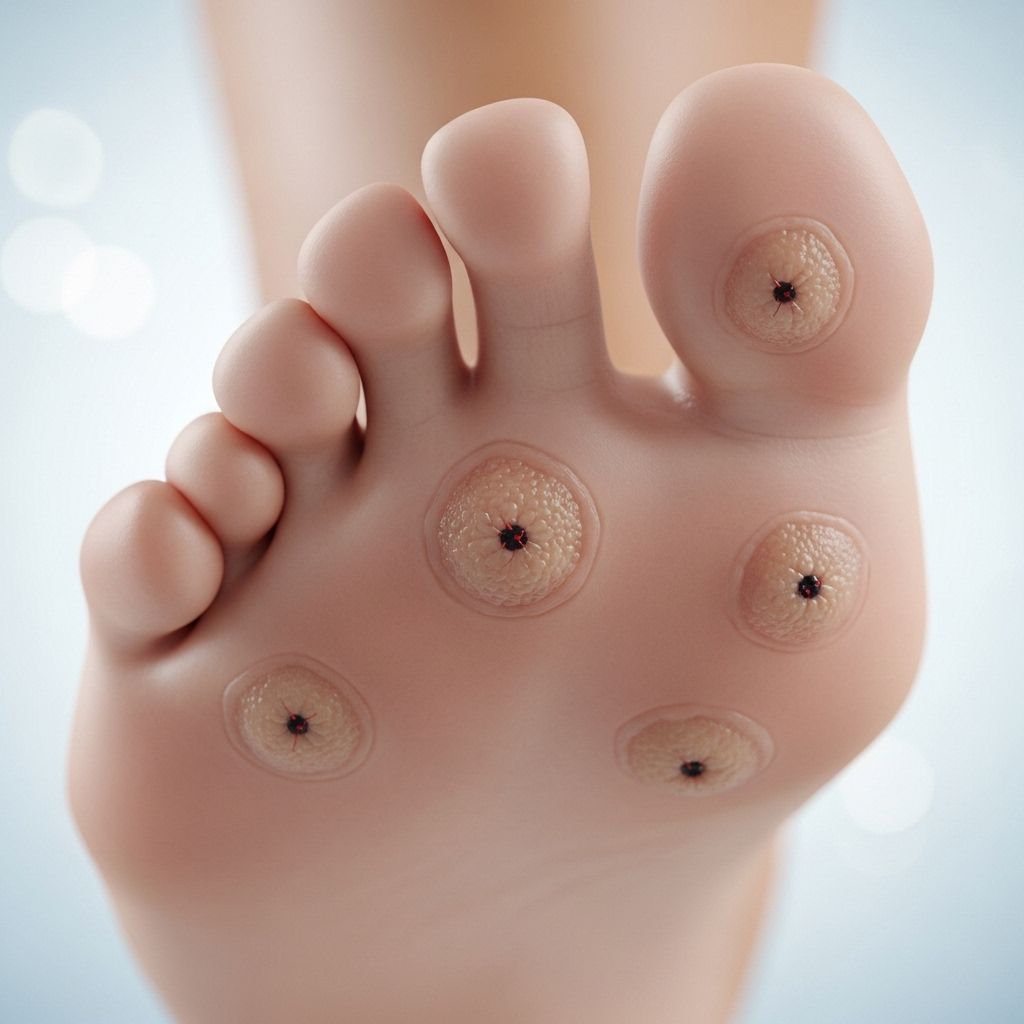
Plantar warts are rough, sometimes painful growths located on the sole of the foot. Although generally harmless, these lesions can cause significant discomfort, especially when pressure is applied while walking or standing. This comprehensive guide explores the nature of plantar warts, their symptoms, causes, risk factors, diagnostic criteria, when to seek a health care provider, and tips for prevention.
Overview
Plantar warts are small, grainy or rough growths that develop most commonly on the weight-bearing areas of your foot—typically the heel or the ball of the foot. Due to constant pressure, the wart can be pressed further inward under a hard layer of skin (a callus), potentially causing pain.
These warts are caused by human papillomavirus (HPV). The virus enters through tiny breaks or cuts on the underside of the foot. While plantar warts are not a serious health concern and are unlikely to cause long-term medical problems, they can be persistent and bothersome. Most will go away on their own, especially in children, but some individuals may require medical intervention for removal or symptom relief.
Symptoms
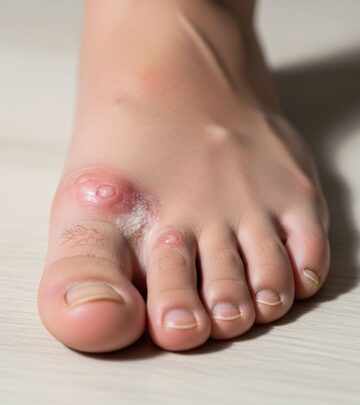
The signs and symptoms of plantar warts typically include:
- Small, rough, flesh-colored growths on the underside (plantar surface) of the foot, often at the base of toes or the heel.
- On brown and black skin, the wart might appear lighter or darker than the surrounding tissue.
- Thickened skin (callus) over a specific spot on the sole, indicating the wart is being pushed inward by foot pressure.
- Black pinpoints within the wart, commonly known as “wart seeds.” These are small, clotted blood vessels inside the wart tissue.
- A cluster of growths on the foot’s sole—sometimes called mosaic warts when warts appear in a group.
- A growth that disrupts the normal lines and ridges of the skin on the foot.
- Pain or tenderness when standing or walking, especially if the wart forms on a weight-bearing area.
In some cases, plantar warts may be mistaken for other skin conditions such as corns or calluses; however, the presence of black dots and the disruption of regular skin lines help differentiate warts.
Visual Signs Table
| Feature | Description |
|---|---|
| Color | Skin-toned, lighter, or darker patches. Sometimes yellowish or brownish on the sole |
| Texture | Rough, thickened, often grainy |
| Location | Base of toes, heel, or ball of the foot |
| Black Dots | Present (clotted capillaries) |
| Pain | Tenderness or pain while walking or standing |
When to See a Doctor
While most plantar warts are not dangerous, there are situations where it’s important to consult a healthcare provider:
- The wart or growth is painful, bleeding, or changes in color or shape.
- You’ve tried self-treatment but the wart persists, multiplies, or frequently recurs.
- Pain interferes with your daily activities or ability to walk.
- You have diabetes, poor sensation in your feet, or other underlying foot problems.
- Your immune system is weakened due to immune-suppressing drugs, HIV/AIDS, or other conditions that compromise immune function.
- There is uncertainty about whether the lesion is a wart or a different growth, such as a corn, callus, or tumor.
Causes
Plantar warts are induced by infection with certain strains of human papillomavirus (HPV). This virus gains access to the deepest layers of skin through tiny cuts, wounds, or weak spots on the bottom of the foot. Not all strains of HPV cause warts, and only some cause plantar warts.
- HPV thrives in warm, moist environments like communal showers, locker rooms, and swimming pool areas.
- Infection does not occur via inoculation through the bloodstream but requires direct contact with the affected skin or contaminated surfaces.
Most people who come into contact with HPV don’t necessarily develop warts—factors like immune system response and the thickness of the skin impact susceptibility.
Transmission Methods
- Direct skin-to-skin contact with someone who has a wart.
- Walking barefoot on wet, contaminated surfaces (e.g., public showers, pool decks).
- Sharing personal items (towels, socks, shoes) with someone carrying HPV.
- Touching your own wart and then another part of the foot or someone else’s skin.
Risk Factors
Though anyone can develop plantar warts, several factors increase risk:
- Age: Most common in children and teenagers due to increased exposure and thinner, more vulnerable skin.
- Weakened immune systems: Individuals with HIV/AIDS, those undergoing immunosuppressive therapy, or those with autoimmune diseases are at higher risk.
- Frequenting communal wet areas: Swimming pools, gyms, and public showers provide environments where HPV flourishes.
- History of warts or existing breaks in the skin from other skin conditions (e.g., eczema), which facilitate viral entry.
Complications
The majority of plantar warts are harmless and self-limiting, especially in otherwise healthy individuals. However, some complications can arise:
- Pain-related gait changes: Discomfort from the wart may cause you to alter how you walk or stand, potentially leading to muscle or joint pain in feet, legs, or back.
- Wart multiplication: Untreated plantar warts can grow in clusters or spread to new areas of the foot.
- Secondary infections: Picking or scratching at a wart increases risk for bacterial infection or further skin breakdown.
Prevention
While not all plantar warts are preventable, following these strategies can reduce risk:
- Avoid walking barefoot in public communal areas, especially showers, gyms, and pool decks.
- Keep feet dry and clean. Change socks daily and let shoes air out between uses.
- Wear “shower shoes” or flip-flops in locker rooms or public bathrooms.
- Do not share personal foot items such as shoes, socks, and towels with others.
- Promptly treat and cover any cuts or abrasions on the feet.
- Avoid touching or picking at warts—if you have one, wash hands after contact and keep it covered.
Self-Care and Management
Minor plantar warts can often be managed at home:
- Over-the-counter treatments: Most OTC products use salicylic acid preparations to soften and gradually remove the wart. Apply as directed and protect skin around the wart.
- Pumice stones or emery boards: Gently filing the callused skin can be helpful—never use the same tool on healthy skin.
- Keep affected area clean and dry.
- If pain or spreading occurs, or if your immune system is weakened, consult a healthcare provider rather than attempting self-removal.
Diagnosis
Health care providers can usually diagnose plantar warts based on appearance and clinical presentation. In some cases, diagnosis may involve:
- Physical examination: Inspecting the growth, checking for skin line disruption and black dots.
- Paring the lesion with a scalpel: Removing the top layer to identify blood vessels (black dots) or to differentiate warts from calluses/corns.
- Biopsy: Rarely needed, but can help confirm diagnosis if the lesion is atypical or if skin cancers are suspected.
Who Gets Plantar Warts?
Plantar warts are widespread and can affect people of any age, but the following populations are more susceptible:
- Children and teenagers, due to higher exposure to shared surfaces and more vulnerable skin.
- Individuals with weakened immune systems (HIV/AIDS, transplant recipients, chemotherapy patients).
- Those with a history of warts or broken skin on the feet.
- People who regularly use public showers or swim facilities.
Frequently Asked Questions (FAQs)
Are plantar warts contagious?
Yes, plantar warts are contagious. They can spread through direct contact with the wart or indirectly via contaminated surfaces, socks, shoes, or towels.
Will plantar warts go away on their own?
In many cases, especially in healthy children, plantar warts can resolve without treatment over months to a few years. However, persistent, painful, or spreading warts may require intervention.
Are plantar warts dangerous?
Plantar warts are usually harmless and present a cosmetic or comfort concern rather than a health threat. Complications arise primarily if the wart is persistently painful, gets infected, or disrupts walking mechanics.
How can I distinguish a plantar wart from a corn or callus?
Plantar warts often disrupt normal skin ridges and have black dots (clotted vessels). Pressing directly on a wart tends to cause pain, while calluses are usually only painful under direct pressure over a bony area. If in doubt, consult a healthcare provider.
When should a child with plantar warts see a doctor?
If a child experiences pain, difficulty walking, worsening of the wart, or there’s uncertainty about diagnosis, consult a healthcare provider. Special care is needed for children with immune system issues or chronic conditions like diabetes.
References
- This guide is based on expert consensus and current information from sources including Mayo Clinic, Cleveland Clinic, and Harvard Medical School.
References
- https://www.health.harvard.edu/diseases-and-conditions/plantar-warts-options-for-treating-this-common-foot-condition
- https://ada.com/conditions/plantar-warts/
- https://pediatricorthopedics.com/plantar-warts-causes-and-treatments/
- https://www.mayoclinic.org/diseases-conditions/plantar-warts/symptoms-causes/syc-20352691
- https://my.clevelandclinic.org/health/diseases/24899-plantar-warts
- https://www.mayoclinic.org/diseases-conditions/plantar-warts/diagnosis-treatment/drc-20352697
- https://www.footcaremd.org/foot-and-ankle-conditions/toes/plantar-warts
- https://www.thefeetpeople.com.au/symptoms-we-treat/plantar-warts/
- https://www.webmd.com/skin-problems-and-treatments/understanding-plantar-warts-basics
- https://my.clevelandclinic.org/health/diseases/15045-warts
Read full bio of Sneha Tete