Pinched Nerve: Symptoms, Causes & Complete Treatment Guide
Understanding nerve compression: from symptoms to recovery strategies
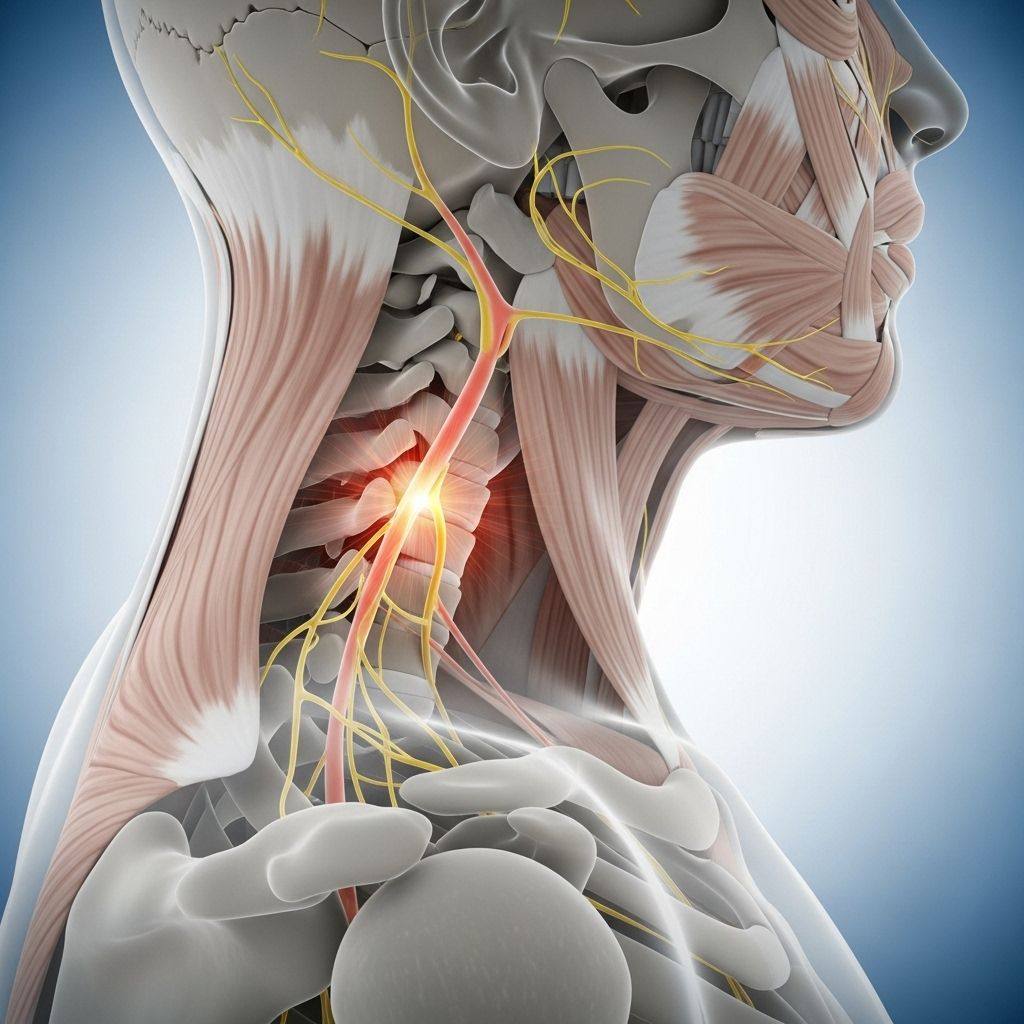
A pinched nerve occurs when excessive pressure, known medically as compression, is applied to a nerve by the surrounding tissues in your body. These tissues can include bones, cartilage, muscles, tendons, or ligaments that press against the nerve, disrupting its normal function. This pressure interferes with the nerve’s ability to transmit signals properly, leading to a range of uncomfortable and sometimes debilitating symptoms that can affect your daily life and overall well-being.
When a nerve experiences compression, it cannot function optimally. The result is often a cascade of symptoms including pain, tingling sensations, numbness, or weakness in the affected area. These symptoms can vary significantly depending on which nerve is compressed and the severity of the compression. Understanding the mechanisms behind nerve compression, recognizing the warning signs, and knowing when to seek medical attention are crucial steps in managing this common medical condition effectively.
Understanding Nerve Compression
Nerve compression represents a specific type of damage or injury to a nerve or group of nerves within your body. The condition develops when surrounding structures exert too much pressure on a nerve, preventing it from functioning correctly. Nerves are particularly vulnerable in areas where they must travel through narrow anatomical spaces, such as tunnels or canals within joints, where there is minimal soft tissue available to cushion and protect them from external pressure.
The compression can occur in various ways depending on the location and surrounding structures. In some cases, a herniated spinal disk may compress a nerve root as it exits the spine, causing pain that radiates along the nerve pathway. In other instances, swelling from inflammation, repetitive motion injuries, or structural changes in bones and joints can gradually increase pressure on nerves over time, leading to chronic symptoms that worsen without proper intervention.
When a nerve experiences compression for only a brief period, there is typically no permanent damage to the nerve tissue. Once the pressure is relieved through rest, position changes, or other interventions, nerve function generally returns to normal relatively quickly. However, when compression persists over an extended period, it can lead to chronic pain and potentially permanent nerve damage that may require more aggressive treatment approaches.
Common Symptoms of a Pinched Nerve
The symptoms associated with a pinched nerve can manifest in various ways, and their severity often depends on the degree of compression and the specific nerve affected. Recognizing these symptoms early can help you seek appropriate treatment before the condition worsens or becomes chronic.
One of the most characteristic symptoms is a sensation of pins and needles, often described as a prickling or tingling feeling in the affected area. This abnormal sensation, known medically as paresthesia, occurs because the compressed nerve cannot transmit sensory information properly. Many people also experience numbness, where an area loses sensation entirely or feels significantly less sensitive to touch, temperature, or pressure.
Pain is another hallmark symptom of nerve compression. This pain can present as sharp, shooting sensations that radiate along the nerve pathway, or it may manifest as a persistent, dull ache that affects a broader area. The pain associated with pinched nerves often intensifies with certain movements or positions that increase pressure on the affected nerve. Interestingly, many people find that their symptoms worsen during sleep, possibly due to prolonged periods of remaining in positions that compress the nerve.
Weakness in the muscles supplied by the compressed nerve is also common, particularly in cases of moderate to severe compression. This weakness can affect your ability to perform everyday tasks, such as gripping objects, walking, or maintaining balance. The weakness develops because the nerve can no longer effectively transmit signals from your brain to the muscles it controls.
A frequently experienced but often overlooked symptom is the sensation of a limb “falling asleep.” This temporary form of nerve compression occurs when poor positioning while sitting or lying down pinches a nerve briefly. The tingling, numbness, and discomfort typically resolve quickly once you change position and relieve the pressure on the nerve.
Where Pinched Nerves Occur in the Body
Pinched nerves can develop in numerous locations throughout your body, though certain areas are more susceptible due to their anatomical structure and the demands placed on them during daily activities. Understanding these common locations can help you identify potential nerve compression issues more quickly.
Spinal Nerve Compression
The spine is one of the most common sites for pinched nerves, particularly where nerve roots exit the spinal cord through small openings between vertebrae. When inflammation or pressure affects these nerve roots, it can cause symptoms that radiate far beyond the compression site. This condition is known as radiculopathy, and its symptoms depend on which section of the spine is affected.
Cervical radiculopathy occurs when a nerve in the neck region becomes compressed, causing pain that may radiate from the neck into the shoulder, arm, hand, or fingers. This type of nerve compression can result from herniated disks, bone spurs, or degenerative changes in the cervical spine. People with cervical radiculopathy often report shooting pain, numbness, or weakness that follows a specific pattern corresponding to the compressed nerve.
Lumbar radiculopathy involves compression of nerves in the lower back region. This compression frequently causes pain that radiates from the lower back down through the buttocks and into the leg and foot, following the pathway of the sciatic nerve. This condition is commonly referred to as sciatica and represents one of the most prevalent forms of nerve compression affecting millions of people worldwide.
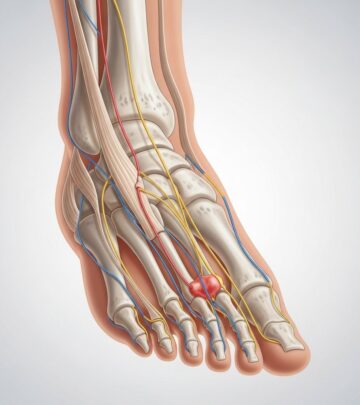
Peripheral Nerve Compression
Beyond the spine, several peripheral nerves are prone to compression due to their location near joints and their passage through narrow anatomical spaces. Carpal tunnel syndrome represents perhaps the most well-known example of peripheral nerve compression. This condition develops when the median nerve becomes compressed as it passes through the carpal tunnel in the wrist, resulting in pain, numbness, and tingling in the hand and fingers.
Cubital tunnel syndrome occurs when the ulnar nerve becomes compressed at the elbow, causing symptoms in the forearm, hand, and fingers, particularly the ring and little fingers. Similarly, radial tunnel syndrome involves compression of the radial nerve near the elbow, leading to pain and weakness in the forearm and hand. These conditions often develop gradually due to repetitive motions, prolonged pressure, or structural abnormalities in the affected area.
Root Causes and Contributing Factors
Understanding what causes nerve compression is essential for both prevention and treatment. Multiple factors and conditions can lead to the development of pinched nerves, ranging from acute injuries to chronic medical conditions that gradually increase pressure on nerves over time.
Structural Changes and Injuries
Herniated disks represent a leading cause of spinal nerve compression. These disks, which serve as cushions between vertebrae in your spine, can slip out of their normal position or develop bulges that protrude into the space where nerves exit the spinal canal. This protrusion creates direct pressure on nerve roots, causing pain and other symptoms that radiate along the affected nerve pathway.
Bone spurs, which are overgrowths of bone tissue, commonly develop as a result of osteoarthritis and the natural aging process. As cartilage in joints wears away over time, the body may respond by forming these bony projections. When bone spurs develop near nerve pathways, they can narrow the spaces through which nerves pass, creating compression and associated symptoms.
Acute injuries from accidents, falls, or sports activities can cause immediate nerve compression through several mechanisms. Direct trauma may cause swelling in tissues surrounding a nerve, or it may result in structural damage to bones, ligaments, or muscles that then press against nearby nerves. Even after the initial injury heals, residual scar tissue or altered anatomy can continue to compress nerves.
Medical Conditions
Rheumatoid arthritis, an autoimmune condition characterized by chronic joint inflammation, significantly increases the risk of nerve compression. The persistent inflammation associated with this disease causes swelling in tissues around joints, which can compress nearby nerves. Additionally, the joint damage that occurs with rheumatoid arthritis can alter normal anatomy in ways that increase pressure on nerves.
Diabetes mellitus affects nerves through multiple mechanisms. Beyond the direct nerve damage known as diabetic neuropathy, diabetes can cause tissue swelling and inflammation that contributes to nerve compression. People with diabetes are particularly susceptible to developing carpal tunnel syndrome and other compression neuropathies.
Thyroid disease, particularly hypothyroidism, has been strongly associated with an increased risk of carpal tunnel syndrome and other nerve compression syndromes. The mechanisms underlying this association are not completely understood but may involve fluid retention and tissue swelling that accompany thyroid dysfunction.
Lifestyle and Occupational Factors
Repetitive motion injuries have become increasingly common in our modern work environment. Activities that involve performing the same movements repeatedly, such as typing on a keyboard, working on an assembly line, or using vibrating tools, can cause inflammation in tendons and other soft tissues. This inflammation increases pressure on nearby nerves, potentially leading to compression syndromes like carpal tunnel syndrome.
Obesity contributes to nerve compression through increased mechanical stress on joints and nerves throughout the body. Excess body weight places additional pressure on weight-bearing joints and can compress nerves in multiple locations. Weight loss often leads to significant improvement in nerve compression symptoms, highlighting the important relationship between body weight and nerve health.
Extended periods of bed rest, whether due to illness, surgery, or injury, can lead to nerve compression. When lying in one position for prolonged periods, pressure on nerves can gradually increase, particularly in areas like the elbows, wrists, or legs where nerves pass close to the surface or through narrow spaces.
Pregnancy represents a temporary but significant risk factor for nerve compression. As the developing baby grows, the increasing size and weight can exert pressure on various organs and structures, including nerves. Hormonal changes during pregnancy also cause fluid retention and tissue swelling, which can contribute to conditions like carpal tunnel syndrome that often resolve after delivery.
Risk Factors for Developing a Pinched Nerve
Certain factors increase your likelihood of experiencing nerve compression at some point in your life. Understanding these risk factors can help you take preventive measures and recognize when you might be particularly vulnerable to developing a pinched nerve.
Age is a significant risk factor, as the natural degenerative changes that occur in bones, joints, and disks over time make nerve compression more likely. The development of bone spurs, disk degeneration, and arthritis all increase with advancing age, creating more opportunities for nerves to become compressed.
Your occupation plays a crucial role in determining your risk level. Jobs that require repetitive motions, prolonged periods in awkward positions, or exposure to vibration significantly increase the likelihood of developing nerve compression. Office workers who spend hours typing, construction workers who use vibrating tools, and assembly line workers who repeat the same motions thousands of times daily are all at elevated risk.
Genetic factors may predispose some individuals to nerve compression. Some people are born with naturally narrower anatomical passages through which nerves must travel, making them more susceptible to compression when any additional swelling or structural change occurs. Family history of conditions like carpal tunnel syndrome suggests a genetic component to susceptibility.
Previous injuries to an area can create lasting changes in tissue structure or scar tissue formation that increases the risk of future nerve compression in that location. Even after an injury appears to have healed completely, subtle anatomical changes may persist that make nerves more vulnerable to compression.
When to Seek Medical Care
While many cases of pinched nerves resolve with conservative self-care measures like rest and over-the-counter pain relievers, certain situations warrant professional medical evaluation and treatment. Knowing when to seek medical care is crucial for preventing permanent nerve damage and ensuring optimal recovery.
You should consult a healthcare professional if your symptoms persist for several days despite rest and self-care measures. When symptoms do not improve or continue to worsen over time, it indicates that the nerve compression is not resolving on its own and may require more targeted intervention.
Severe or progressively worsening pain that interferes with your daily activities or sleep definitely requires medical attention. Similarly, if you develop significant weakness in the affected area that impairs your ability to perform normal tasks, you should seek evaluation promptly, as this may indicate more severe nerve compression that could lead to permanent damage if left untreated.
Any loss of bladder or bowel control associated with back pain or nerve compression symptoms constitutes a medical emergency requiring immediate attention, as this may indicate severe spinal cord compression that requires urgent treatment to prevent permanent damage.
Diagnostic Approaches
When you visit a healthcare provider for evaluation of a suspected pinched nerve, they will employ several approaches to identify the source and severity of the nerve compression. The diagnostic process typically begins with a thorough physical examination of the affected area, during which your provider will check for muscle weakness, assess your reflexes, and ask detailed questions about the sensations you are experiencing.
Your provider will carefully evaluate the distribution of your symptoms, as nerve compression typically causes symptoms that follow specific anatomical patterns corresponding to the compressed nerve. By understanding where you feel pain, numbness, or tingling, they can often pinpoint which nerve is affected and where the compression is occurring.
In many cases, additional diagnostic tests are necessary to confirm the diagnosis and determine the exact cause of nerve compression. Nerve conduction studies measure how quickly electrical impulses travel through your nerves, helping identify areas where nerve function is impaired. Electromyography assesses the electrical activity in your muscles, which can reveal whether muscle weakness is due to nerve compression.
Imaging studies such as X-rays, magnetic resonance imaging (MRI), or computed tomography (CT) scans provide detailed views of bone and soft tissue structures. These tests can identify herniated disks, bone spurs, tumors, or other structural abnormalities that may be compressing nerves. MRI is particularly valuable because it provides excellent visualization of soft tissues, including nerves, disks, ligaments, and muscles.
Treatment and Management Options
Treatment for pinched nerves varies depending on the location, severity, and underlying cause of the compression. Most people recover successfully with conservative treatment approaches that focus on relieving pressure on the affected nerve and allowing it to heal naturally.
Conservative Treatment
Rest is often the first and most important treatment recommendation. Avoiding or modifying activities that worsen your symptoms allows inflammation to subside and gives the compressed nerve time to recover. This may involve taking breaks from repetitive motions, adjusting your workspace ergonomics, or temporarily avoiding certain physical activities.
Over-the-counter pain relievers and anti-inflammatory medications can help reduce pain and inflammation associated with nerve compression. These medications can make you more comfortable while other treatment measures take effect, though they should be used according to package directions and medical advice.
Physical therapy plays a crucial role in treating many cases of nerve compression. A physical therapist can teach you specific exercises to strengthen muscles, improve flexibility, and relieve pressure on compressed nerves. They may also use modalities such as heat, ice, ultrasound, or electrical stimulation to reduce pain and inflammation.
Splinting or bracing can be particularly helpful for peripheral nerve compression syndromes like carpal tunnel syndrome. These devices hold the affected joint in a neutral position that minimizes pressure on the nerve, especially during sleep when people often unconsciously adopt positions that worsen nerve compression.
Advanced Treatment
When conservative measures do not provide adequate relief, or when nerve compression is severe, more advanced treatments may be necessary. Corticosteroid injections can reduce inflammation around the compressed nerve, providing significant pain relief and potentially allowing the nerve to heal. These injections are particularly useful for spinal nerve compression and some peripheral compression syndromes.
In cases where conservative treatment fails to provide relief or when there is evidence of progressive nerve damage, surgery may be recommended. Surgical procedures aim to relieve pressure on the compressed nerve by removing or altering the structures causing compression. For example, carpal tunnel release surgery enlarges the carpal tunnel to reduce pressure on the median nerve, while spinal surgery might remove herniated disk material or bone spurs compressing nerve roots.
Prevention Strategies
While not all cases of nerve compression can be prevented, certain strategies can significantly reduce your risk of developing a pinched nerve. Maintaining good posture during daily activities reduces unnecessary stress on your spine and peripheral nerves. When sitting at a desk, ensure your workstation is ergonomically designed with your computer screen at eye level, your feet flat on the floor, and your wrists in a neutral position while typing.
Taking regular breaks from repetitive activities allows tissues to recover and reduces inflammation that can lead to nerve compression. If your work involves repetitive motions, try to vary your tasks throughout the day and perform stretching exercises during breaks to maintain flexibility and reduce tension in muscles and tendons.
Maintaining a healthy weight reduces mechanical stress on joints and nerves throughout your body. Regular exercise helps control weight while also strengthening muscles that support joints and maintain proper alignment, reducing the likelihood of nerve compression.
Strengthening and flexibility exercises specifically targeting areas prone to nerve compression can provide better support and protection for vulnerable nerves. A balanced exercise program that includes both strength training and stretching is ideal for maintaining nerve health and preventing compression.
Frequently Asked Questions
Q: How long does it take for a pinched nerve to heal?
A: Most pinched nerves resolve within a few days to a few weeks with proper rest and conservative treatment. However, recovery time varies depending on the severity of compression and the underlying cause. More severe cases or those involving chronic compression may require several months of treatment or even surgical intervention for complete recovery.
Q: Can a pinched nerve cause permanent damage?
A: Yes, if a nerve remains compressed for an extended period without treatment, it can lead to permanent nerve damage. This is why it’s important to seek medical attention if symptoms persist or worsen despite self-care measures. Early intervention significantly improves the likelihood of complete recovery without lasting effects.
Q: Is it safe to exercise with a pinched nerve?
A: This depends on the location and severity of your nerve compression. Generally, you should avoid activities that worsen your symptoms, but gentle stretching and low-impact exercises may actually help in some cases. Always consult with your healthcare provider or physical therapist before beginning any exercise program when dealing with a pinched nerve.
Q: What’s the difference between a pinched nerve and a herniated disk?
A: A herniated disk is a specific condition where the soft inner material of a spinal disk protrudes through its outer layer. A pinched nerve is a broader term describing nerve compression that can be caused by many different factors, including but not limited to herniated disks. Essentially, a herniated disk is one possible cause of a pinched nerve.
Q: Can stress cause a pinched nerve?
A: While stress itself doesn’t directly cause nerve compression, it can contribute to muscle tension and poor posture that increase your risk of developing a pinched nerve. Chronic stress may cause you to hold your body in tense positions, particularly in the neck and shoulders, which can gradually lead to nerve compression in susceptible areas.
Q: Are there any home remedies that can help relieve pinched nerve symptoms?
A: Yes, several home remedies can provide relief for mild pinched nerve symptoms. These include applying ice or heat to the affected area, getting adequate rest, maintaining proper posture, performing gentle stretching exercises, and taking over-the-counter anti-inflammatory medications. However, if symptoms persist beyond a few days, professional medical evaluation is recommended.
References
- https://www.webmd.com/pain-management/compressed-nerves
- https://www.kuh.ku.edu.tr/mayo-clinic-care-network/mayo-clinic-health-information-library/diseases-conditions/pinched-nerve
- https://www.amerikanhastanesi.org/mayo-clinic-care-network/mayo-clinic-health-information-library/diseases-conditions/pinched-nerve
- https://my.clevelandclinic.org/health/diseases/6481-pinched-nerves
- https://www.mayoclinic.org/diseases-conditions/pinched-nerve/diagnosis-treatment/drc-20354751
- https://www.mayoclinic.org/diseases-conditions/peripheral-nerve-injuries/symptoms-causes/syc-20355631
- https://sportsmedicine.mayoclinic.org/condition/radiculopathy/
- https://www.mayoclinic.org/diseases-conditions/sciatica/symptoms-causes/syc-20377435
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/sciatica-and-radiculopathy-peculiar-names
Read full bio of medha deb