Hand-Foot-and-Mouth Disease: Diagnosis, Treatment and Care
Learn about the diagnosis, treatment, and at-home care for hand-foot-and-mouth disease to support quick recovery and comfort.
Hand-Foot-and-Mouth Disease: Diagnosis, Treatment and Home Care
Hand-foot-and-mouth disease is a highly contagious viral infection most often affecting infants and children under 5, but teens and adults can also contract the illness. While generally mild and self-limiting, the disease can cause significant discomfort due to its characteristic mouth sores and skin rash. Understanding how providers diagnose the disease, what treatments are available, and how to manage symptoms at home is vital to ensuring comfort and prevention of complications.
Diagnosis
Diagnosis of hand-foot-and-mouth disease is typically carried out with a thorough physical examination and review of symptoms. Your healthcare provider will evaluate:
- Age of the patient: The condition is most common in children younger than 5 years but can occur at any age.
- Symptoms: Providers will ask about fever, sore throat, malaise, irritability, and appetite loss.
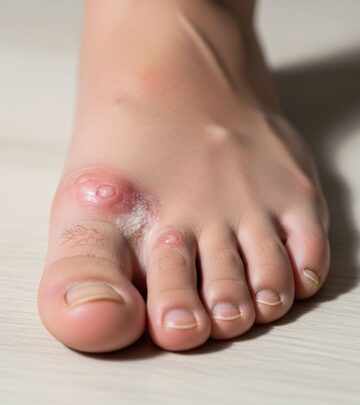
- Appearance of rash or sores: The presence and pattern of blister-like lesions on the hands, feet, in the mouth, or occasionally on the buttocks or legs helps distinguish this disease from other viral rashes.
In most cases, these steps are sufficient for diagnosis. However, if there is diagnostic uncertainty or a severe presentation, further testing may be done. These may include:
- Throat swab: A sample from the throat may be collected to help identify the virus responsible for the infection.
- Stool sample: Sometimes a stool sample is also analyzed because some viruses that cause hand-foot-and-mouth disease can be detected in feces.
Lab results can confirm the specific virus (often Coxsackievirus), but since the disease is usually mild, laboratory tests are rarely needed in typical cases.
Treatment
There is no specific antiviral treatment for hand-foot-and-mouth disease. The illness generally resolves on its own within 7 to 10 days. Treatment is focused on relieving symptoms, especially mouth pain and fever, and keeping the child comfortable and hydrated.
Over-the-counter Pain Relief
- Acetaminophen (Tylenol, etc.) or ibuprofen (Advil, Motrin IB, etc.) can help reduce fever and general discomfort.
- Do not give aspirin to children or teenagers. Aspirin is associated with Reye’s syndrome, a rare but serious illness that can affect children recovering from viral infections.
Topical Oral Anesthetics
- Products containing topical oral anesthetics (as found in some lozenges and throat sprays) can relieve mouth sore pain.
- Do not give lozenges to children under 4 years old, due to choking hazard.
- Do not use benzocaine—a common anesthetic ingredient in throat sprays—for kids under 2 years old; it can cause a rare, serious condition called methemoglobinemia.
Other Medications
- Prescription medications are generally not required.
- Antibiotics are ineffective since the illness is caused by viruses, not bacteria.
Self-Care and Home Management
The biggest concerns during hand-foot-and-mouth disease are mouth pain (which can interfere with eating and drinking) and the risk of dehydration. Home care measures play a crucial role in keeping patients comfortable while symptoms run their course.
Tips to Relieve Mouth Soreness and Support Nutrition
- Suck on ice pops or ice chips.
- Eat ice cream, sherbet, or similar cold, soft foods.
- Sip cold drinks (such as water or milk) frequently.
- Sip warm drinks like mild tea for those who find warmth soothing.
- Avoid acidic foods and drinks (citrus fruits, fruit juices, soda), which can make mouth pain worse.
- Choose soft foods that are easy to swallow and require little chewing, such as yogurt, pudding, or mashed potatoes.
For children old enough to rinse without swallowing:
- Rinsing with warm salt water several times a day may help ease mouth pain and inflammation. (Mix about 1/2 teaspoon of salt in 1 cup of warm water.)
Hydration and Rest
- Keep your child well hydrated. Offer fluids regularly; dehydration can occur if mouth pain prevents adequate fluid intake.
- Allow for extra rest and downtime. Fatigue is common during the illness.
How to Prevent Spreading the Infection
Hand-foot-and-mouth disease is highly contagious, especially in group childcare environments and during summer or early fall. The virus is spread by contact with:
- Respiratory droplets (coughing, sneezing)
- Person-to-person contact
- Touching contaminated objects or surfaces
- Stool from an infected individual (prompt hygiene after diaper changes is important)
To protect others and reduce transmission risks:
- Practice frequent and thorough hand-washing, especially after restroom use or helping a sick child.
- Disinfect toys and frequently touched surfaces regularly.
- Keep children home from daycare, school, or group settings while they have a fever, open sores, or are feeling unwell.
- Avoid close contact (hugging, kissing, sharing cups/utensils) during the contagious period.
When to Seek Medical Attention
While hand-foot-and-mouth disease is most often mild, complications (such as dehydration) can occasionally arise. Contact your healthcare provider if:
- Your child is unable or unwilling to drink fluids because of mouth pain.
- Your child has signs of dehydration such as decreased urination, dry mouth, crying without tears, or lethargy.
- Symptoms worsen or persist beyond 7 to 10 days.
- There is a high, persistent fever or if the patient appears unusually drowsy, irritable, or unwell.
Very rarely, complications like viral meningitis or encephalitis (infection affecting the brain) can occur, especially in those with weakened immune systems. These are medical emergencies, and you should seek help if there are signs of severe headache, neck stiffness, seizure, or confusion.
Table: Comparison of Symptom Management and Prevention
| Aspect | Recommended Approach | Precautions |
|---|---|---|
| Pain relief | Acetaminophen, ibuprofen (not aspirin) | Check dosages for age; avoid aspirin entirely in children |
| Mouth sores | Topical oral anesthetics; warm salt water rinses; soft and cold foods | No lozenges for <4 years; no benzocaine sprays for <2 years |
| Hydration | Encourage regular cold/warm fluids, popsicles, and soft foods | Monitor for signs of dehydration |
| Symptom duration | Typically 7–10 days | Seek care if worsening or not improving |
| Contagion prevention | Frequent handwashing, disinfecting surfaces, home isolation | Keep child home until fever and open sores resolve |
Frequently Asked Questions (FAQs)
Q: How long does hand-foot-and-mouth disease last?
A: Symptoms usually clear up within 7 to 10 days. The contagious period is greatest during the first week, but the virus can sometimes be shed in stool for several weeks after recovery.
Q: Can adults get hand-foot-and-mouth disease?
A: While most common in children younger than 5, adults (including parents, teachers, and caregivers) can also contract the virus, although symptoms often tend to be milder.
Q: What can I do to help my child eat or drink when mouth sores make it painful?
A: Offer cold and soft foods (ice pops, yogurt, sherbet), encourage frequent sips of water or cold fluids, and avoid acidic or salty foods that may sting. If your child is unable to swallow or shows signs of dehydration, consult a healthcare provider immediately.
Q: Should my child stay home from school or daycare?
A: Yes. Children with fever or open blisters should stay home to avoid spreading the infection. Your healthcare provider or local health authority can offer specific guidance depending on symptoms and local policies.
Q: Is it possible to get hand-foot-and-mouth disease more than once?
A: Yes. Several different viruses can cause the illness. Immunity to one virus doesn’t protect you from others, so reinfection is possible.
Key Takeaways
- Hand-foot-and-mouth disease is a mild, highly contagious viral illness primarily affecting children.
- No specific cure exists; care is focused on symptom relief, hydration, and preventing the spread of infection.
- Home remedies and supportive care are usually sufficient, but parents must watch out for dehydration or any signs of complications.
- Good hygiene is critical to limit transmission, especially in childcare and school settings.
- Contact a healthcare provider if symptoms are severe or if your child cannot stay hydrated.
For further support or specific concerns about symptoms, always reach out to your healthcare provider for guidance tailored to your child’s situation.
References
- https://www.mayoclinic.org/diseases-conditions/hand-foot-and-mouth-disease/diagnosis-treatment/drc-20353041
- https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-q-and-a-hand-foot-and-mouth-disease/
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/hand-foot-and-mouth-common-in-children
- https://www.youtube.com/watch?v=Tv1v-rMiK4A
- https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-minute-hand-foot-and-mouth-disease-in-kids/
- https://www.kuh.ku.edu.tr/mayo-clinic-care-network/mayo-clinic-health-information-library/definitions/hand-foot-and-mouth-disease
- https://www.mayoclinic.org/diseases-conditions/hand-foot-and-mouth-disease/diagnosis-treatment/drc-20353041?p=1
Read full bio of Sneha Tete