Graves’ Disease: Symptoms, Causes, and Management
Exploring Graves' disease: an autoimmune disorder impacting thyroid function, symptoms, causes, risk factors, and treatments in detail.

Graves’ disease is a complex autoimmune disorder that leads to an overactive thyroid, also known as hyperthyroidism. As the most common cause of hyperthyroidism, Graves’ disease triggers a range of physical and emotional symptoms and requires targeted management strategies.
This comprehensive guide explains what Graves’ disease is, explores its symptoms and causes, outlines associated risk factors and complications, and reviews current treatment approaches.
What is Graves’ Disease?
Graves’ disease is an autoimmune condition in which the immune system erroneously attacks the thyroid gland—a small butterfly-shaped organ at the base of the neck, below the Adam’s apple. This abnormal immune response stimulates the thyroid to produce excessive amounts of thyroid hormones, speeding up the body’s metabolism and affecting numerous organ systems.
Graves’ disease is the leading cause of hyperthyroidism and most commonly impacts women and individuals under 40 years old.
Role of the Thyroid in the Body
- Located at the base of the neck.
- Produces hormones that regulate metabolism, energy production, heart rate, and temperature.
- Excess hormone production leads to widespread effects—overactivity can accelerate processes throughout the body.
Symptoms of Graves’ Disease
The hallmark of Graves’ disease is hyperthyroidism, or an overactive thyroid gland. Symptoms may develop gradually and vary in intensity. Some symptoms are specific to thyroid hormone excess, while others result from unique immune system effects.
Common Signs and Symptoms
- Anxiety and irritability
- Unintentional weight loss, despite normal or increased appetite
- Heat sensitivity; increased sweating
- Rapid or irregular heartbeat (palpitations)
- Nervousness or restlessness
- Hand tremors
- Fatigue and muscle weakness
- Difficulty sleeping
- Frequent bowel movements
- Thinning skin and brittle hair
- Menstrual changes (reduced flow or irregular cycles in women)
- Swelling at the base of the neck (goiter)
Specific Symptoms: Graves’ Ophthalmopathy
About one-third of people with Graves’ disease experience Graves’ ophthalmopathy, a condition affecting the eyes:
- Bulging eyes (exophthalmos)
- Redness and swelling of the eyes
- Dry or gritty feeling
- Double vision
- Light sensitivity
- Pressure or pain in the eyes
- In rare cases, vision loss
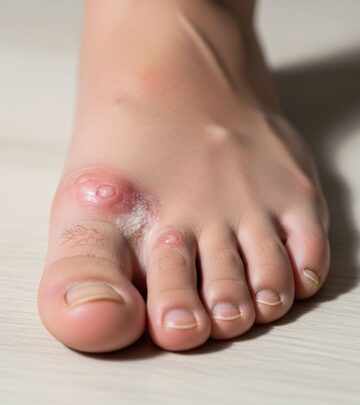
Skin Symptoms: Graves’ Dermopathy
Less commonly, individuals may develop Graves’ dermopathy:
- Thick, reddened skin often found on the shins or tops of the feet
When to See a Doctor
- If you experience unintentional weight loss, rapid heartbeat, abnormal sweating, swelling at the base of your neck, or other signs of hyperthyroidism, schedule a medical consultation.
- Early diagnosis and treatment reduce the risk of long-term complications.
Causes of Graves’ Disease
Graves’ disease is triggered by the immune system mistakenly invading the thyroid gland. The primary cause is the production of abnormal antibodies—specifically, thyroid-stimulating immunoglobulin (TSI)—that mimic the action of thyroid-stimulating hormone (TSH), causing the thyroid to produce excessive hormones.
While the exact reason for this autoimmune attack is unknown, genetic and environmental factors play key roles.
Key Factors Contributing to Graves’ Disease
- Genetic predisposition: Family history of Graves’ disease or other autoimmune disorders increases risk.
- Sex hormones: Women are significantly more likely to develop Graves’ disease than men.
- Environmental triggers: Stress, infection, pregnancy, and smoking may contribute to disease development or trigger immune responses.
Risk Factors for Graves’ Disease
Several factors can increase susceptibility to Graves’ disease:
- Family history: Having relatives with Graves’ disease or other autoimmune diseases.
- Sex and age: Women under age 40 are most commonly affected.
- Autoimmune predisposition: Existing autoimmune conditions (type 1 diabetes, rheumatoid arthritis, lupus).
- Thyroid disorders: Past or current issues with thyroid function.
- Smoking: Raises risk, especially of eye problems.
- Pregnancy: Hormonal changes may elevate risk.
- Stress or infection: May act as triggers in genetically predisposed individuals.
Complications of Graves’ Disease
If left untreated, Graves’ disease can result in serious complications affecting multiple body systems:
- Heart disorders: Rapid, irregular heartbeat can lead to heart failure, increased blood pressure, and risk of stroke.
- Thyroid eye disease: Vision impairment due to pressure and inflammation behind the eyes.
- Osteoporosis: Excess thyroid hormone accelerates bone loss.
- Pregnancy complications: Increased risk of miscarriage, preterm birth, poor fetal growth, and maternal heart failure.
- Thyroid storm: A rare, sudden, and life-threatening exaggeration of hyperthyroid symptoms, often requiring emergency care.
Diagnosis of Graves’ Disease
Diagnosis combines clinical evaluation of symptoms with laboratory and imaging studies.
- Physical examination: Identifies characteristic signs.
- Blood tests: Measure levels of thyroid hormones (T3, T4) and TSH.
- Antibody tests: Detect thyroid-stimulating immunoglobulins (TSI).
- Radioactive iodine uptake test: Evaluates thyroid activity.
- Thyroid ultrasound: Imaging study to assess gland structure and rule out nodules.
Treatment of Graves’ Disease
Managing Graves’ disease focuses on restoring normal thyroid hormone levels and preventing complications. Treatment options depend on age, disease severity, presence of eye disease, and individual medical characteristics.
Main Treatment Approaches
- Radioactive iodine therapy: Administered orally, radioactive iodine selectively destroys overactive thyroid cells, shrinking the gland and reducing hormone production. Most patients require lifelong thyroid hormone replacement therapy afterwards.
- Anti-thyroid medications: Prescription drugs such as methimazole and propylthiouracil block the thyroid’s ability to make hormones. Methimazole is generally preferred due to lower risk of serious side effects, except early in pregnancy when propylthiouracil may be considered. Side effects include rash, joint pain, and rarely liver failure.
- Surgery (thyroidectomy): Surgical removal of the thyroid gland may be recommended when other treatments are unsuitable or have failed. Surgery offers a permanent cure but necessitates lifelong hormone replacement therapy.
- Beta-blockers: These medications, though not targeting the thyroid itself, can help control rapid heart rate and other symptoms while primary treatments take effect.
Treating Graves’ Ophthalmopathy
- Mild eye symptoms: Lubricating eye drops, sunglasses, and cool compresses.
- Moderate to severe cases: Corticosteroids, immunosuppressive therapy, and sometimes surgery to relieve pressure or correct vision issues.
Treating Graves’ Dermopathy
- Topical corticosteroids applied to affected skin areas.
- Compression therapy and other supportive care.
Lifestyle and Home Remedies
- Routine monitoring and ongoing healthcare to adjust treatments as needed.
- Quitting smoking to reduce risk of eye problems.
- Managing stress through relaxation techniques or support groups.
- Balanced diet and regular exercise to preserve bone health and cardiovascular function.
Living with Graves’ Disease
Effective management of Graves’ disease depends on personalized care and regular monitoring. Treatment plans may be tailored over time as symptoms change or new complications arise. Early and consistent treatment improves quality of life and reduces risk of long-term health issues.
Frequently Asked Questions (FAQs)
What is the main cause of Graves’ disease?
The main cause is the production of abnormal antibodies by the immune system that overstimulate the thyroid gland.
Who is most likely to develop Graves’ disease?
Women under age 40 and those with a family history of autoimmune diseases are at highest risk.
Can Graves’ disease affect other parts of my body?
Yes. It may impact the eyes, skin, heart, bones, and can complicate pregnancy.
Is Graves’ disease curable?
Treatments can control symptoms and reverse the effects, though lifelong hormone replacement may be needed if the thyroid gland is destroyed or removed.
What should I do if I suspect Graves’ disease?
Seek evaluation from a healthcare professional. Diagnosis is based on symptoms, physical exam, and specific blood and imaging tests.
How is Graves’ ophthalmopathy managed?
Mild cases may only require eye drops or protective measures, while severe cases might need immunosuppressive drugs or surgical intervention.
Does Graves’ disease recur after treatment?
Medications may control symptoms, but relapse can occur. Definitive therapies such as radioactive iodine or surgery generally prevent recurrence, but require hormone replacement.
Summary Table: Graves’ Disease At a Glance
| Aspect | Details |
|---|---|
| What is it? | Autoimmune disorder causing thyroid overactivity (hyperthyroidism) |
| Main symptoms | Anxiety, weight loss, rapid heartbeat, bulging eyes, sweating, tremors |
| Risk factors | Women under 40, family history, smoking, pregnancy, other autoimmune diseases |
| Complications | Heart disorders, bone loss, vision issues, pregnancy problems |
| Treatment options | Radioactive iodine, anti-thyroid drugs, surgery, beta-blockers, immunosuppressives for eye disease |
| Long-term management | Lifelong monitoring; may need hormone replacement |
Resources and Support
- Clinical expertise: Centers such as Mayo Clinic provide specialized care and ongoing research for Graves’ disease management.
- Insurance: Consult with your provider regarding coverage, referrals, or requirements before accessing specific treatment centers.
- Patient support: Support groups and educational resources can help patients and families navigate the challenges associated with Graves’ disease.
Key Takeaways
- Graves’ disease is a common cause of hyperthyroidism, resulting from an autoimmune attack on the thyroid gland.
- Symptoms range from anxiety and weight loss to bulging eyes and skin changes.
- Prompt medical evaluation and treatment are essential to prevent serious complications.
- Multiple therapies exist, including medication, radioactive iodine, and surgery; management is tailored to each patient.
- Ongoing research continues to improve strategies for diagnosis and care.
References
- https://www.mayoclinic.org/diseases-conditions/graves-disease/diagnosis-treatment/drc-20356245
- https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-minute-graves-disease-when-the-thyroid-is-overactive/
- https://www.mayoclinic.org/diseases-conditions/graves-disease/care-at-mayo-clinic/mac-20356248
- https://www.youtube.com/watch?v=mhYeuD_Z3Po
- https://www.mayoclinic.org/diseases-conditions/graves-disease/symptoms-causes/syc-20356240
- https://www.mayoclinic.org/diseases-conditions/hyperthyroidism/symptoms-causes/syc-20373659
- https://www.mayoclinic.org/diseases-conditions/hyperthyroidism/diagnosis-treatment/drc-20373665
- https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/thyroid-disease-symptoms-and-treatment
- https://my.clevelandclinic.org/health/diseases/15244-graves-disease
- https://www.mayoclinic.org/diseases-conditions/graves-disease/doctors-departments/ddc-20356247
Read full bio of Sneha Tete