Gout: Symptoms, Causes, Risk Factors, and Effective Management
An in-depth guide to understanding, preventing, and managing gout—a common and complex form of arthritis.
Gout is a common and complex form of arthritis that can affect anyone. Characterized by sudden and severe attacks of pain, swelling, redness, and tenderness in joints—most often the big toe—gout results from an accumulation of urate crystals caused by high levels of uric acid in the blood. This article provides a detailed overview of gout, including its symptoms, causes, risk factors, complications, diagnostic methods, and management strategies to help individuals understand and cope with this chronic condition.
Overview
Known as a form of inflammatory arthritis, gout is marked by sudden and excruciating pain episodes primarily in the big toe joint. However, it can affect any joint, including the ankles, knees, elbows, wrists, and fingers. Gout symptoms tend to develop quickly and can last from a few days to several weeks, with intervals of remission in between attacks.
While gout is most commonly seen in men, women become increasingly susceptible after menopause. Prompt recognition and effective management of gout are key to preventing joint damage and improving quality of life.
Symptoms
Gout attacks, or flares, often occur suddenly and at night. They are characterized by the following features:
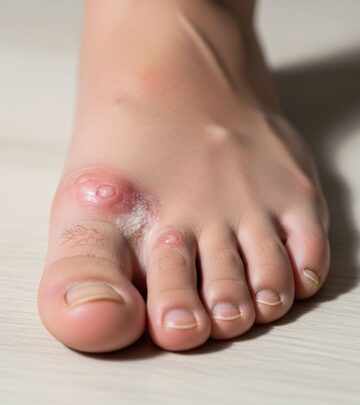
- Intense joint pain, usually starting in the big toe, but can affect ankles, knees, elbows, wrists, or fingers.
- Lingering discomfort that can last from days to weeks after the acute pain subsides. Subsequent attacks may last longer and affect more joints.
- Inflammation and redness around the affected joint.
- Swelling, warmth, and tenderness—the joint often feels hot and is extremely sensitive to touch, sometimes even to the weight of a bedsheet.
- Limited range of motion in the affected joint, especially if gout progresses unchecked.
It is important to note that not all joint pain or swelling is due to gout. Conditions with similar presentations, such as pseudogout and septic arthritis, require different treatments, making accurate diagnosis essential.
When to See a Doctor
- Seek prompt medical attention if you experience sudden, intense joint pain and swelling. Early treatment can help reduce the risk of complications.
- If you develop a fever and a hot, inflamed joint, seek immediate help. These symptoms may indicate infection or septic arthritis, which require urgent care.
Causes
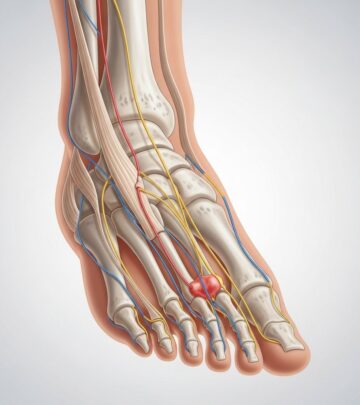
The root cause of gout is an accumulation of urate crystals in joints and surrounding tissues. These sharp, needlelike crystals form when the blood contains high levels of uric acid (hyperuricemia). Uric acid is a waste product formed by the breakdown of substances called purines, naturally found in the body, and in certain foods and drinks.
- Normally, uric acid is dissolved in the blood, filtered by the kidneys, and excreted in urine.
- If the body produces too much uric acid, or the kidneys fail to eliminate enough, uric acid levels rise.
- Excess uric acid leads to crystal formation, which trigger inflammation and acute pain in the affected joints.
Common foods and drinks associated with increased uric acid levels include:
- Red meats and organ meats (liver, kidney, etc.)
- Seafood (sardines, anchovies, shellfish)
- Sugary beverages, especially those sweetened with fructose
- Alcohol, particularly beer and spirits
Risk Factors
Several factors elevate the risk of developing gout by contributing to higher levels of uric acid in the body:
- Diet: Consuming excessive red meats, organ meats, certain seafood, and high-fructose drinks can raise uric acid levels.
- Alcohol consumption: Especially beer and spirits, which interfere with uric acid elimination and increase production.
- Obesity: Larger body mass increases the turnover of purines, thus producing more uric acid; it also impairs the kidneys’ ability to filter uric acid efficiently.
- Medical conditions: Unmanaged high blood pressure, diabetes, metabolic syndrome, heart and kidney diseases, and some types of cancers can contribute to gout risk.
- Medications: Diuretics (‘water pills’), low-dose aspirin, some immunosuppressant drugs, and certain medications for hypertension can raise uric acid levels.
- Genetic factors: A family history of gout increases personal risk.
- Age and sex: Men are more likely to develop gout at a younger age; women’s risk increases after menopause due to lower estrogen levels, which help eliminate uric acid.
- Recent trauma or surgery: These stressors can sometimes trigger a gout attack.
- Dehydration: Not drinking enough water reduces uric acid clearance.
Complications
If left untreated or poorly managed, gout can lead to more serious health problems, including:
- Recurrent gout: Some people may only experience one gout attack, while others have frequent recurrences that gradually damage the affected joints.
- Tophi formation: Untreated gout may cause deposits of urate crystals under the skin, called tophi. These can become swollen, tender, and sometimes infected. Tophi often appear in the fingers, hands, feet, elbows, or Achilles tendons.
- Joint destruction: Chronic gout can erode and destroy joints, resulting in reduced mobility and permanent damage.
- Kidney stones: Uric acid crystals may collect in the urinary tract, forming stones that can cause pain and kidney damage.
- Chronic kidney disease: Persistent high uric acid levels elevate the risk for kidney impairment over time.
Prevention
Taking proactive steps can help lower uric acid levels, prevent flares, and minimize long-term complications of gout. Preventive strategies include:
- Healthy diet: Focus on fruits, vegetables, whole grains, and lean proteins like low-fat dairy. Limit red meat, organ meats, and high-purine seafood. Avoid sugary beverages and cut back on alcohol.
- Stay hydrated: Drink sufficient water throughout the day; dehydration raises uric acid concentration.
- Maintain a healthy body weight: Gradual weight loss can help lower uric acid. Rapid weight loss, fasting, or very low-calorie diets may increase uric acid temporarily and should be avoided.
- Exercise regularly: Physical activity helps maintain a healthy weight and overall well-being, though joints with active gout flare should be rested.
- Manage medical conditions: Properly control blood pressure, diabetes, and cholesterol through medications and lifestyle choices.
- Discuss medications with your healthcare provider: If you are taking diuretics or other drugs that affect uric acid, talk to your doctor about alternatives where possible.
Diagnosis
Early and accurate diagnosis of gout is crucial for effective management and prevention of complications. Diagnostic approaches include:
- Medical history and symptom assessment: Your healthcare provider will ask about symptoms, frequency, and duration of attacks, as well as risk factors such as diet and family history.
- Physical examination: Inspection and palpation of the affected joint to identify redness, swelling, warmth, and tenderness.
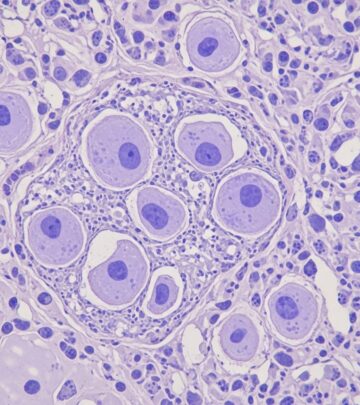
- Joint fluid analysis: Extraction of synovial fluid from the affected joint (arthrocentesis) to look for urate crystals under a microscope. Presence of needle-shaped, negatively birefringent crystals confirms gout.
- Blood tests: Measurement of serum uric acid levels. However, these levels might be normal during a flare or elevated for other reasons, so test results are interpreted in context.
- Imaging: X-rays, ultrasound, or dual-energy CT scans may help detect joint damage or urate crystal deposits, especially in advanced cases.
Treatment
Management of gout focuses on two main goals: treating acute attacks and preventing future flares or complications. Treatment strategies may vary based on symptom frequency, disease severity, and coexisting health conditions. The main approaches include:
Managing Acute Gout Attacks
- Nonsteroidal anti-inflammatory drugs (NSAIDs): These medications, such as ibuprofen, naproxen, or prescription-strength indomethacin, can quickly reduce inflammation and pain. Long-term use should be avoided due to potential side effects.
- Colchicine: An anti-inflammatory medication that is most effective when taken soon after symptoms start. Side effects can include gastrointestinal upset.
- Corticosteroids: Oral or injected corticosteroids (such as prednisone) are another option to relieve inflammation, especially for those who can’t tolerate NSAIDs or colchicine. Prolonged use is generally avoided due to side effects.
Long-term Management and Prevention
- Urate-lowering therapies: Medications such as allopurinol or febuxostat reduce uric acid production, while probenecid increases uric acid excretion.
- Regular monitoring: Periodic blood tests to monitor serum uric acid levels and assess treatment effectiveness. Targets are typically below 6 mg/dL, or even 5 mg/dL for severe or advanced gout.
- Lifestyle changes: Adopting a gout-friendly diet, reducing alcohol and sugary drinks, maintaining hydration, and losing excess weight.
Managing Complications
If complications such as tophi or kidney stones develop, additional medications or surgical interventions may be necessary. Persistent tophi may require surgical removal if they become painful, infected, or interfere with movement.
Living With Gout: Tips for Everyday Life
- Work closely with healthcare professionals to develop a personalized management plan.
- Track your symptoms and triggers with a journal to help identify patterns and avoid flare-ups.
- Prioritize adherence to prescribed medications and recommended lifestyle modifications.
- Exercise regularly but avoid stressing affected joints during flares; opt for low-impact activities like swimming, cycling, or walking.
- Stay informed about your condition, treatments, and potential side effects.
Frequently Asked Questions (FAQs)
Q: What triggers a gout attack?
A: Common triggers include consumption of high-purine foods (red meat, organ meats, certain seafood), excessive alcohol, dehydration, sudden weight loss, trauma, or surgery.
Q: Can gout be cured?
A: Gout is a chronic condition, but symptoms can be effectively managed and flares minimized with the right combination of medications and lifestyle changes. Ongoing management is essential to prevent complications.
Q: Is gout only a problem for older men?
A: While men are more likely to develop gout at a younger age, women can also get gout, especially after menopause when their risk increases.
Q: Are there foods that people with gout should avoid?
A: Yes, it’s advisable to limit red meat, organ meats, high-purine seafood, sugary drinks, and alcohol—particularly beer and spirits. Consuming low-fat dairy, fruits, and vegetables is generally recommended.
Q: How important is hydration in managing gout?
A: Drinking plenty of water helps dilute uric acid levels and supports kidney function, reducing the likelihood of gout attacks and kidney stones.
Q: What are tophi, and what problems can they cause?
A: Tophi are deposits of urate crystals under the skin, usually around joints or tendons. They can lead to pain, swelling, skin ulceration, and infection, and sometimes require surgical removal if severe.
Table: Key Risk Factors for Gout
| Risk Factor | Description | Modifiable? |
|---|---|---|
| Diet | High intake of purine-rich foods (red meat, seafood) and sugary drinks | Yes |
| Alcohol | Especially beer and spirits, which increase uric acid production | Yes |
| Obesity | Increases uric acid production and decreases kidney function | Yes |
| Medical Conditions | High blood pressure, diabetes, kidney disease, metabolic syndrome | Partly |
| Genetics | Family history of gout | No |
| Medications | Diuretics, aspirin, immunosuppressants | Partly |
Key Takeaways
- Gout is a form of arthritis caused by urate crystal deposition due to excess uric acid.
- It causes sudden, severe joint pain, often in the big toe but can affect other joints.
- Diagnosis relies on clinical assessment, joint fluid analysis, and supporting lab or imaging findings.
- Management includes prompt treatment of acute attacks, urate-lowering therapy for long-term control, and lifestyle modifications focused on diet, hydration, and weight management.
- Preventive steps and adherence to prescribed therapies can greatly reduce gout flares and complications.
References
- https://www.mayoclinic.org/diseases-conditions/gout/symptoms-causes/syc-20372897
- https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/gout-diet/art-20048524
- https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-q-and-a-treating-gout-involves-combination-of-lifestyle-changes-medication/
- https://www.youtube.com/watch?v=QXNCYw3A6GU
- https://www.mayoclinic.org/diseases-conditions/pseudogout/symptoms-causes/syc-20376983
- https://www.amerikanhastanesi.org/mayo-clinic-care-network/mayo-clinic-health-information-library/diseases-conditions/gout
- https://communityhealth.mayoclinic.org/featured-stories/gout
- https://www.youtube.com/watch?v=5xAY2T5v5EU
Read full bio of medha deb