Diverticulitis Diet: What to Eat During and After a Flare-Up
Comprehensive guidance on eating strategies to manage, recover from, and prevent diverticulitis flare-ups.
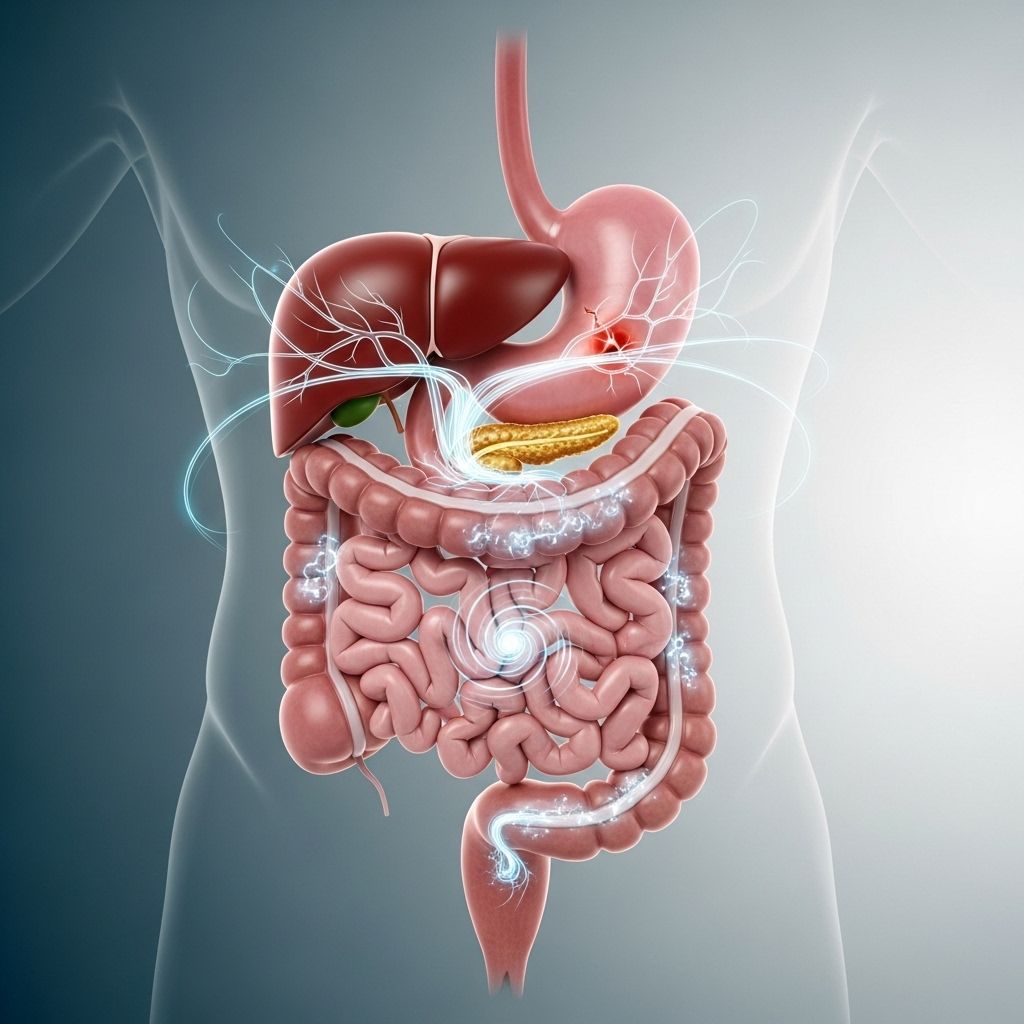
Diverticulitis is a condition characterized by the inflammation or infection of small pouches—called diverticula—that form in the walls of the colon. Managing diverticulitis often includes dietary changes that vary based on whether you are experiencing an active flare-up, recovering, or seeking to prevent future episodes. This comprehensive guide outlines the optimal diet during each stage and provides evidence-based strategies for long-term digestive health.
What is Diverticulitis?
Diverticulitis refers to the inflammation or infection of diverticula in the colon. These pouches can cause sudden abdominal pain, fever, and changes in bowel habits when inflamed. Nutrition plays a vital role in the management and prevention of diverticulitis, and your healthcare professional may adjust your eating plan according to:
- Whether you are currently experiencing a diverticulitis flare-up
- Your stage of recovery
- Your overall risk for recurrence
This adaptive approach is often summarized as the “diverticulitis diet.”
Diet During a Diverticulitis Flare-Up
The main objective of the diet during an acute diverticulitis flare is to rest the digestive tract. In many cases, this begins with a clear liquid diet, especially if the symptoms are severe and hospitalization is required. For mild cases managed at home, a period of clear liquids, followed by low-fiber foods, is standard.
Clear Liquid Diet Phase
Clear liquids are recommended as they are easy to digest and minimize bowel activity. This phase is generally short-term, lasting a few days until symptoms improve. Your diet during this phase may include:
- Broth (chicken, beef, or vegetable)
- Fruit juices without pulp (apple, grape, cranberry)
- Plain water
- Soda and clear sports drinks
- Tea or coffee (without cream or milk)
- Ice pops without fruit or pulp
- Ice chips
- Plain gelatin
- Hard candies
Because a clear liquid diet is low in essential nutrients, your healthcare provider may suggest nutritional supplements to prevent deficiencies during this stage.
Transition to Low-Fiber Diet
Once symptoms begin to improve, you may transition to a low-fiber diet. This phase is also temporary, designed to continue resting the colon while gently reintroducing nutrients.
Examples of low-fiber, easily digestible foods include:
- Canned or cooked fruits without skins or seeds
- Canned or cooked vegetables such as green beans, peas, carrots, and potatoes (no skin)
- Refined grains: white bread, white rice, plain pasta, noodles
- Low-fiber cereals (e.g., Cream of Wheat, cereals made from white or refined flour)
- Eggs
- Fish and poultry
- Dairy: milk, low-fat yogurt, cheese (if tolerated)
- Fruit juice with little or no pulp
Tips during this phase:
- Eat small, frequent meals (5-6 meals a day)
- Include 1-2 ounces of protein and a serving of low-fiber food per meal
- Drink plenty of fluids to prevent dehydration
When to Return to a Regular Diet
Your healthcare professional will guide you on when it is safe to gradually return to your normal diet. Typically, this occurs as symptoms subside and bowel function normalizes. Transition back to a regular diet should be gradual to avoid overwhelming the digestive tract.
Cautions and Monitoring During Flare-Ups
Most people with mild diverticulitis start to feel better within 2–3 days of the diet and appropriate medical management. You should contact your healthcare provider if you:
- Do not improve after several days
- Develop a fever
- Have worsening abdominal pain
- Are unable to keep down clear liquids
These symptoms may indicate complications requiring further medical evaluation or hospitalization.
Risks and Limitations of the Diverticulitis Diet
While short-term clear liquid and low-fiber diets are sometimes necessary for diverticulitis management, remaining on these diets for more than a few days carries risks. Prolonged restriction can lead to:
- Weakness and fatigue
- Nutritional deficiencies
- Other health complications
Therefore, healthcare professionals recommend resuming a normal diet with sufficient fiber and nutrients as soon as it is safe to do so.
Diet to Prevent Diverticulitis Recurrence
Once you have recovered, transitioning to a high-fiber diet is critical for long-term digestive health and minimizing the risk of future diverticulitis attacks. Fiber helps move waste through the colon and prevents constipation and increased pressure, both of which can aggravate diverticula.
Recommended Daily Fiber Intake
| Group | Recommended Daily Fiber (grams) |
|---|---|
| Women | 25 |
| Men | 38 |
These are minimum targets for adults, based on dietary guidelines.
High-Fiber Foods to Include
- Beans and legumes (lentils, chickpeas)
- Whole grain breads and cereals
- Brown and wild rice
- Fruits: apples, bananas, pears, berries
- Vegetables: broccoli, carrots, corn, squash
- Whole wheat pasta
- Nuts and seeds (unless otherwise advised)
Increase your fiber intake slowly to minimize bloating and gas, and ensure you drink plenty of water to help fiber move efficiently through your system.
What About Nuts, Seeds, and Popcorn?
Historically, people with diverticulitis were cautioned to avoid these foods for fear they might lodge in diverticula and cause inflammation. However, current medical evidence finds no link between eating seeds, nuts, or popcorn and an increased risk of diverticulitis. Ask your healthcare professional for individualized advice if you are uncertain.
Additional Lifestyle Tips for Diverticulitis Prevention
- Regular physical activity: Exercise such as brisk walking or swimming supports a healthy colon and regular bowel movements.
- Drink adequate water: Fiber needs water to work effectively in the digestive tract.
- Avoid smoking: Smoking is linked with higher complication rates in diverticular disease.
- Maintain a healthy weight: Excess body fat is related to increased risk for complications.
Speak with your healthcare provider before starting any new exercise or diet plan, particularly if you have ongoing medical concerns.
Sample Meal Plan: Recovery from Diverticulitis Flare-Up
| Stage | Food Options |
|---|---|
| Clear Liquid | Broth, apple juice, gelatin, tea without cream, ice chips |
| Low-Fiber | White bread, eggs, canned peaches (no skin), tender chicken, low-fat yogurt |
| Transition | Gradually add cooked vegetables, small portions of brown rice, ripe bananas |
| Prevention/Normal | Whole grain toast, mixed beans, steamed broccoli, pears with skin, oatmeal |
Frequently Asked Questions (FAQs)
Q: How long should I follow a clear liquid or low-fiber diet during a diverticulitis flare-up?
A: The clear liquid phase generally lasts 2–3 days, until symptoms improve. Low-fiber foods may follow for an additional few days. Always follow your healthcare professional’s advice and return to a regular diet as soon as you are cleared to do so.
Q: Can I ever eat nuts, seeds, or popcorn again with a history of diverticulitis?
A: There is no current scientific evidence that these foods increase the risk of recurrent diverticulitis. Most patients do not need to avoid them unless specifically advised by their doctor.
Q: What if my symptoms do not improve with dietary changes?
A: If your pain worsens, you develop a fever, or cannot tolerate fluids, contact your healthcare provider immediately, as you may require medication or hospitalization.
Q: Are fiber supplements necessary after diverticulitis?
A: If you cannot reach your fiber goals through food alone, your healthcare provider may suggest a fiber supplement. However, most people can meet their needs with a well-rounded, plant-based diet.
Q: How can I add fiber to my diet safely after an episode?
A: Increase fiber foods gradually over several weeks, adding one new high-fiber food at a time and accompanying each addition with extra water to help prevent discomfort.
Practical Tips for Living Well with Diverticulitis
- Work with your healthcare team: Everyone’s situation differs. Individualize your meal plan with the help of a registered dietitian or doctor.
- Keep a food diary: Track your dietary changes and symptoms to identify what works best for you.
- Stay consistent: Make fiber and hydration a daily priority to support long-term digestive comfort.
Key Takeaways
- During an acute diverticulitis episode, follow a clear liquid then low-fiber diet for a few days, under medical supervision.
- Transition to a high-fiber diet as soon as possible for recovery and prevention of recurrence.
- Nuts, seeds, and popcorn are not proven to trigger flare-ups and are generally safe for most people.
- Stay hydrated and physically active to support optimal colon function.
- Seek medical help promptly if symptoms worsen during a flare-up.
References
- https://indygastro.com/wp-content/uploads/2024/10/Diverticulosis-Diet.pdf
- https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/diverticulitis-diet/art-20048499
- https://courtneymedicalgroupaz.com/2022/02/02/diverticulosis-diet-how-to-eat-well-and-feel-good/
- https://newsnetwork.mayoclinic.org/discussion/mayo-clinic-q-and-a-diet-lifestyle-choices-can-lower-risk-of-diverticulosis-developing-into-diverticulitis/
- https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/expert-answers/diverticulitis-diet/faq-20058293
- https://ehr.wrshealth.com/shared/practice-documents/1832434/pf_226_CCF10062010_00000.pdf
- https://www.kuh.ku.edu.tr/mayo-clinic-care-network/mayo-clinic-health-information-library/first-aid/diverticulitis-diet
- https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/low-fiber-diet/art-20048511
- https://health.clevelandclinic.org/what-foods-should-you-eat-and-avoid-on-a-diverticulitis-diet
- https://www.mayoclinic.org/diseases-conditions/diverticulitis/symptoms-causes/syc-20371758
Read full bio of Sneha Tete