Carotid Endarterectomy: Procedure, Risks, Results, and What to Expect
Learn how carotid endarterectomy treats carotid artery disease, lowers stroke risk, and what you can expect before, during, and after surgery.
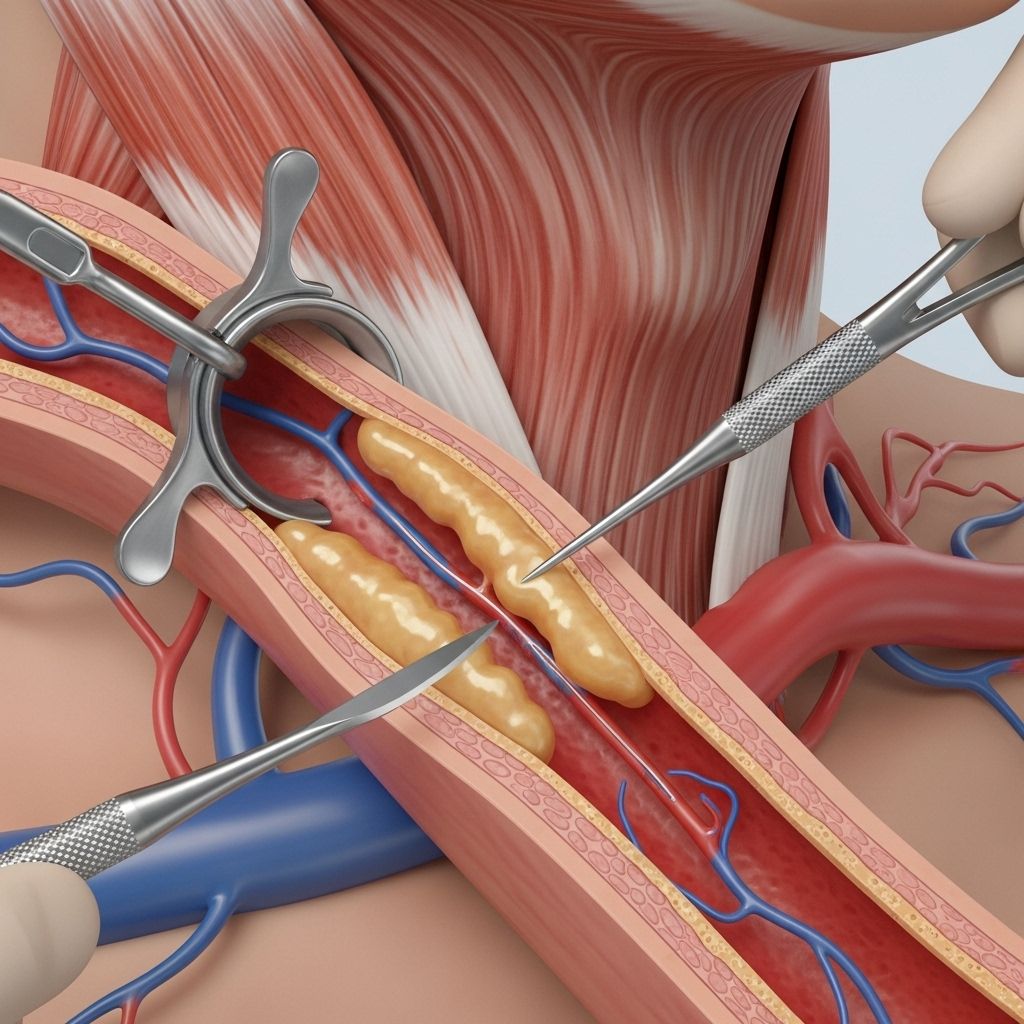
Carotid Endarterectomy
Carotid endarterectomy is a surgical procedure used to treat carotid artery disease, a condition characterized by the buildup of fatty, waxy substances known as plaque inside the carotid arteries. These arteries, located on both sides of the neck, are responsible for transporting oxygen-rich blood to the brain. When plaque accumulates in these vessels—a process called atherosclerosis—it restricts blood flow and increases the risk of stroke. By surgically removing the plaque, carotid endarterectomy aims to restore normal blood circulation and reduce the likelihood of stroke.
Overview
Carotid endarterectomy specifically targets plaque buildup that narrows the carotid arteries. The goal is to prevent major neurological events by improving blood flow and mitigating the threat posed by blood clots or plaque fragments that could block smaller arteries in the brain and cause a stroke. Among various treatment options, carotid endarterectomy is considered especially effective for patients with significant narrowing of the arteries who also have symptoms such as transient ischemic attacks (TIAs) or a recent stroke.
- Carotid arteries are major vessels supplying the brain with oxygenated blood.
- Plaque buildup can severely restrict blood flow and threaten brain health.
- Surgery removes plaque to reduce stroke risk and enhance cerebral circulation.
Why It’s Done
The primary reasons for performing carotid endarterectomy are:
- Prevention of stroke caused by a blocked or severely narrowed carotid artery.
- Treatment of carotid artery disease in patients with symptoms or high-risk plaque accumulation.
- Improvement of blood flow to the brain by eliminating the physical obstruction posed by plaque.
Physicians consider this procedure in individuals who have:
- Already experienced a minor stroke or TIA.
- Carotid arteries narrowed by more than 50–70%.
- High risk for future strokes due to the extent or location of plaque.
In some cases, alternatives such as angioplasty and stenting may be considered, depending on patient health and anatomical factors.
Risks and Complications
Every surgical intervention carries risks. For carotid endarterectomy, these include:
- Stroke (most serious risk), which may occur if a blood clot or fragment of plaque travels to the brain during or after surgery.
- Heart attack caused by stress on the cardiovascular system.
- Nerve injury leading to hoarseness, difficulty swallowing, or numbness in the tongue and face.
- Bleeding and infection at the incision site.
- Re-stenosis (recurrence of artery narrowing over time).
Major morbidity and mortality rates for carotid endarterectomy are reported to be about 1.8% for primary stenosis, with higher complication rates (around 8.5%) in cases of recurrent stenosis. Improved anesthetic and perioperative care have contributed to better outcomes in recent decades. An institutional audit of surgical results is important, as expertise and careful monitoring directly impact safety and success rates.
How You Prepare
Preparation for carotid endarterectomy typically includes:
- Detailed evaluation with physical examination and imaging studies (such as Doppler ultrasound, CT angiography, or MRI) to assess the severity of artery narrowing.
- Review of medical history, especially cardiac and neurological conditions.
- Discussion of risks and benefits with a multidisciplinary team including neurologists, vascular surgeons, and anesthesiologists.
- Instructions for medications, including possible adjustments to anticoagulant or antiplatelet drugs before surgery.
- Preoperative fasting and other standard surgical protocols.
Your care team works to ensure that you are fully informed about the procedure and recovery expectations. Safety protocols are designed to lower the risk of complications and maximize positive outcomes.
What You Can Expect
During the Procedure
- The procedure may be done under local or general anesthesia.
- The surgeon makes an incision along the front of the neck to access the carotid artery.
- A temporary shunt may be used to maintain blood flow to the brain while the artery is being repaired.
- The surgeon then opens the artery and removes the plaque responsible for the blockage.
- After removal, the artery is repaired with stitches or a patch (which may use a vein from the patient or synthetic material) to close the incision.
- In eversion carotid endarterectomy, the carotid artery is cut and turned inside out so plaque can be removed en bloc, after which the artery is reattached.
| Step | Description |
|---|---|
| Incision | Surgeon cuts along the front of the neck |
| Access | Carotid artery is exposed |
| Temporary Shunt | Blood flow maintained to the brain (optional) |
| Plaque Removal | Plaque buildup is carefully extracted |
| Artery Repair | Artery is closed with stitches or patch |
| Closure | Incision is sealed; recovery begins |
After the Procedure
- Hospital stay: Most patients spend a day or two recovering in the hospital.
- Monitoring: Nurses and doctors observe for signs of bleeding, nerve injury, stroke, or other complications.
- Pain management: Pain is typically mild and controlled with medications.
- Recovery instructions: Activities may be temporarily restricted; instructions for wound care and follow-up appointments are provided.
- Long-term care: Continued management of risk factors for atherosclerosis (such as blood pressure, cholesterol, smoking) is important for preventing future problems.
Results
Carotid endarterectomy is generally successful at restoring blood flow in the carotid artery. Most patients experience a significant reduction in their risk of future stroke, particularly those with symptomatic carotid artery disease or moderate to severe stenosis. The best outcomes are observed at centers with experienced multidisciplinary teams and strict protocols for patient selection, surgical technique, and perioperative care.
Some key points about results:
- Stroke risk reduction: Marked decrease in future stroke incidence.
- Low mortality and complication rates at experienced institutions.
- Recurrence: A small percentage of patients may experience stenosis recurrence or require additional interventions.
- Long-term monitoring and lifestyle modification are essential for sustained benefits.
Alternatives: Carotid Angioplasty and Stenting
For some patients, carotid angioplasty and stenting may be considered as an alternative:
- A catheter is threaded into the artery via the groin and advanced to the blockage site.
- A tiny balloon is inflated to widen the artery, and a stent is placed to keep it open.
- This technique may be preferred for individuals with high surgical risk.
- Nationwide trials, including the CREST trial, have evaluated the safety and effectiveness of both options.
| Feature | Endarterectomy | Angioplasty/Stenting |
|---|---|---|
| Approach | Open neck surgery | |
| Anesthesia | General or local | |
| Recovery time | Several days | |
| Ideal for | Healthy, lower surgical risk |
Clinical Studies and Innovations
Ongoing research and clinical trials at major centers such as Mayo Clinic aim to further refine the safety, efficiency, and outcomes of carotid endarterectomy. Innovations in surgical technique, anesthesia, perioperative monitoring, and adjunctive pharmacological therapy continue to lower complication rates and improve patient experience.
Care and Experience at Mayo Clinic
Mayo Clinic’s multidisciplinary approach integrates neurology, neurosurgery, vascular and endovascular surgery, radiology, and cardiovascular medicine. Collaboration among specialists ensures personalized care and access to advanced technology and techniques. Highlights include:
- Experienced team of surgeons and support staff.
- Comprehensive preoperative evaluation and individualized treatment planning.
- Access to advanced imaging and minimally invasive options.
- Recognition for excellence in heart, vascular, and neurological care.
The high volume of carotid endarterectomy procedures performed at Mayo Clinic translates to greater expertise and superior patient outcomes.
Frequently Asked Questions (FAQs)
What is carotid endarterectomy?
Carotid endarterectomy is a surgical procedure to remove plaque buildup from the carotid arteries in the neck to restore blood flow to the brain and reduce the risk of stroke.
How do I know if I need carotid endarterectomy?
Your medical team may recommend this surgery if imaging tests show significant narrowing of your carotid arteries, especially if you have had symptoms such as TIA or minor stroke.
What are the risks of carotid endarterectomy?
The main risks include stroke during or shortly after the procedure, nerve injury, heart attack, bleeding, infection, and possible artery narrowing recurrence.
How long does recovery take?
Most people spend 1–2 days in the hospital. Full recovery may take several weeks, depending on overall health and any complications that arise.
Can carotid artery disease recur after surgery?
Yes, but recurrence rates are low—especially with good control of cholesterol, blood pressure, and lifestyle factors. Regular monitoring by your physician is vital.
Are there alternatives to carotid endarterectomy?
Yes, carotid angioplasty and stenting offer minimally invasive alternatives for certain patients, especially those with high surgical risk or challenging anatomy.
What can I do to prevent carotid artery disease?
- Control blood pressure and cholesterol.
- Stop smoking.
- Eat a healthy diet rich in fruits, vegetables, and whole grains.
- Stay active and maintain a healthy weight.
Conclusion
Carotid endarterectomy remains a cornerstone in the prevention and treatment of stroke related to carotid artery disease. Surgical advances, experienced multidisciplinary care, and ongoing research have enhanced safety and outcomes, making it a reliable option for selected patients. Alternative procedures such as angioplasty and stenting expand the possibilities for individualized care. Patients are encouraged to discuss all available options, risks, and follow-up needs with their medical team to achieve optimal long-term health.
References
- https://pubmed.ncbi.nlm.nih.gov/9095622/
- https://www.mayoclinic.org/tests-procedures/carotid-endarterectomy/care-at-mayo-clinic/pcc-20393385
- https://www.mayoclinic.org/tests-procedures/carotid-endarterectomy/about/pac-20393379
- https://www.mayoclinic.org/diseases-conditions/carotid-artery-disease/care-at-mayo-clinic/mac-20360532
- https://www.mayoclinic.org/diseases-conditions/carotid-artery-disease/diagnosis-treatment/drc-20360527
- https://www.mayoclinic.org/diseases-conditions/carotid-artery-disease/multimedia/carotid-endarterectomy/img-20006850
- https://www.mayoclinichealthsystem.org/locations/eau-claire/services-and-treatments/cardiac-surgery/conditions-and-treatments/carotid-artery-disease
- https://www.mayoclinic.org/tests-procedures/carotid-angioplasty-and-stenting/about/pac-20385111
- https://www.mayoclinic.org/tests-procedures/carotid-endarterectomy/multimedia/vid-20078203
Read full bio of Sneha Tete