Arteriovenous Malformation (AVM): Symptoms, Causes, and Risks
Understand arteriovenous malformations—causes, symptoms, risk factors, types, and when to seek medical care.
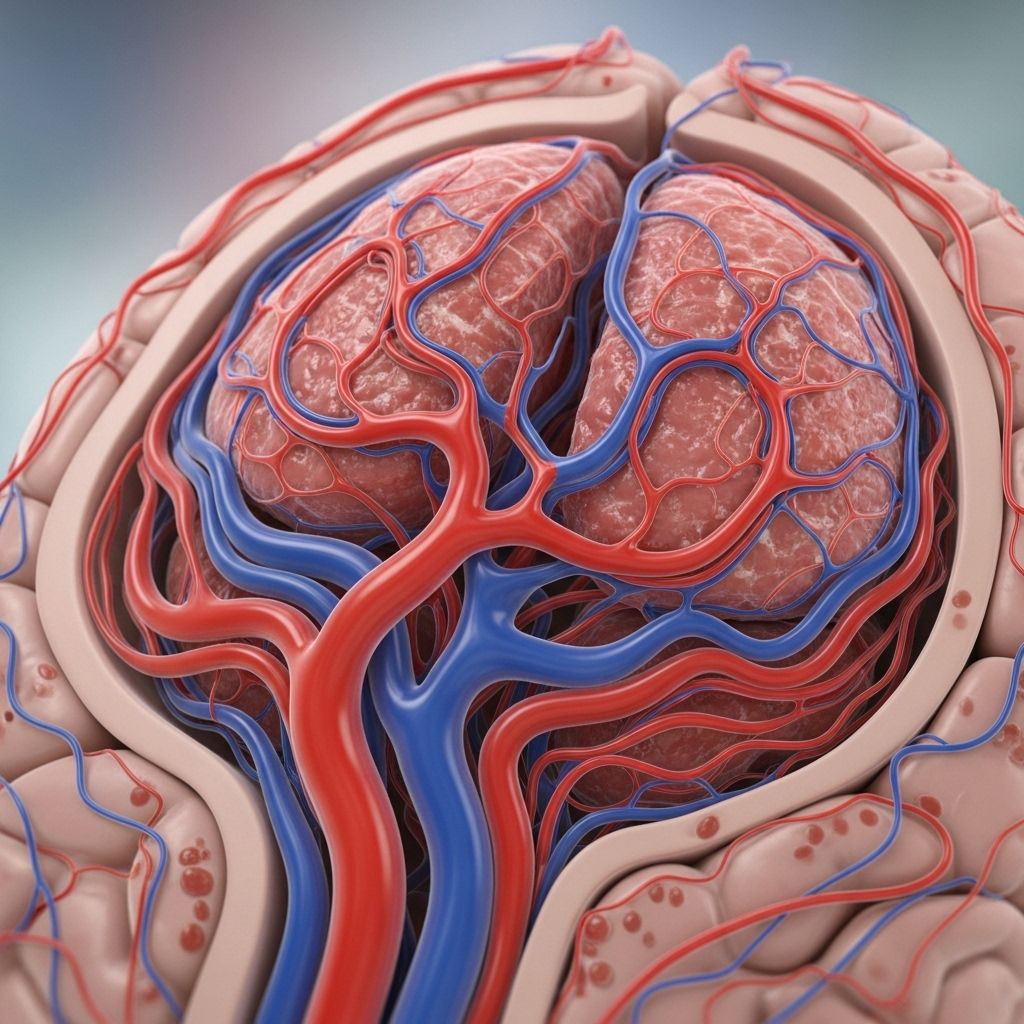
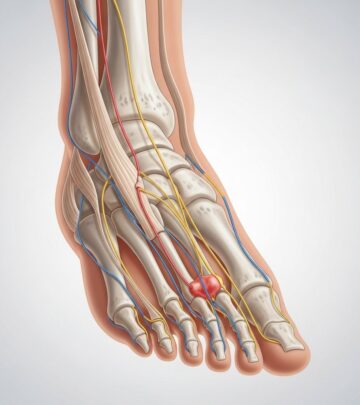
Arteriovenous malformations (AVMs) are abnormal tangles of blood vessels connecting arteries and veins, bypassing the capillary system. This anomaly disrupts normal blood flow and oxygen circulation, most often affecting the brain or spinal cord. While many AVMs are present from birth, they can remain unrecognized for years, only becoming apparent through severe neurological symptoms or complications. This comprehensive guide explores the definition, symptoms, causes, risk factors, complications, types of AVMs, and advice on when to seek medical attention.
Overview
An arteriovenous malformation (AVM) is a cluster of abnormally intertwined blood vessels where arteries connect directly to veins, often resulting in high-pressure blood flow that bypasses the normal capillary network. The majority of AVMs are congenital, meaning they typically form during fetal development, although their precise cause remains unknown. AVMs are rare but serious—especially when located within the central nervous system, as they carry an elevated risk of bleeding or neurological complications.
- Common Locations: Brain, spinal cord, but can develop in other organs
- Main risk: Interruption of oxygen supply to surrounding tissues
- Prevalence: Relatively rare, with brain AVMs found in approximately 1 in every 700 people
Symptoms
Symptoms of AVM vary depending on its size, location, and whether complications such as bleeding have occurred. Some individuals may never develop noticeable symptoms, and AVMs are sometimes discovered incidentally during imaging for unrelated conditions. Nevertheless, AVMs—especially those in the brain or spinal cord—often present with neurological symptoms, which may be sudden or progress gradually over time.
Common symptoms include:
- Bleeding (hemorrhage): Often the first sign, particularly with brain AVMs; can lead to sudden, severe headache or neurological deficit
- Seizures
- Headaches: Persistent or severe headache, sometimes with specific features depending on AVM location
- Progressive neurological problems: Such as weakness, numbness, or problems with movement or coordination
- Vision difficulties: If AVM affects areas related to sight
- Speech or language difficulties: Including problems with understanding or producing speech
- Paralysis or loss of coordination: Depending on the brain or spinal cord region involved
- Back pain and limb weakness: More common in spinal cord AVMs
- Numbness, tingling, or sudden pain in limbs (spinal cord AVMs)
- Trouble walking, urinating, or with bowel control (spinal cord involvement)
Symptoms may appear at any age, but often begin in young adulthood or childhood in more severe cases. In some AVM types, symptoms may arise during pregnancy or with physical exertion that raises blood pressure.
When to Seek Medical Care
Immediate medical attention is necessary if any of the following symptoms appear suddenly:
- Sudden, severe headache
- Seizure with no prior history
- Weakness, numbness, or paralysis on one side
- Sudden visual disturbances
- Problems understanding or expressing speech
- Severe, sudden back pain (for spinal AVMs)
Prompt evaluation is particularly important because these may indicate a bleeding AVM, which is a medical emergency.
Causes
The exact cause of arteriovenous malformations is unknown. Most AVMs are categorized as congenital, originating during embryonic or fetal development, likely due to abnormal blood vessel formation in the brain, spinal cord, or other organs.
Key points about AVM causes:
- Congenital origin: Most AVMs develop before birth, likely due to a mishap in vascular development
- Genetic association: Some AVMs (especially in the brain) are associated with hereditary hemorrhagic telangiectasia (HHT), a genetic disorder affecting blood vessel formation
- Acquired AVMs: In rare cases, AVMs develop later in life, potentially associated with trauma or injury, but these are less common
In healthy circulation, arteries deliver oxygen-rich blood, which gradually slows as it passes through branching arterioles and tiny capillaries, allowing oxygen to diffuse into tissues. Blood then returns via veins to the heart and lungs. In AVMs, this network is bypassed; blood moves rapidly from arteries to veins, depriving nearby tissues of oxygen and increasing pressure on veins, which can lead to rupture.
Risk Factors
AVMs are rare and typically occur without an identifiable risk factor. However, a few variables are linked to increased risk:
- Family history: Inherited genetic disorders like hereditary hemorrhagic telangiectasia can increase risk
- Congenital factors: Most AVMs are present at birth, but the specific triggers in prenatal development remain unclear
- Gender: Spinal AVMs occur equally in men and women, but most AVMs show no significant gender bias
- History of nervous system injury: Rarely, CNS injuries may raise the likelihood of developing vascular malformations
Complications
AVMs can lead to serious health complications, particularly due to their effects on the central nervous system:
- Bleeding (hemorrhage): The most common and dangerous complication, especially in brain AVMs. The risk of bleeding increases after the first hemorrhage
- Stroke: Disruption of blood flow can result in brain tissue damage, stroke, or death
- Brain or spinal cord damage: Recurrent or significant bleeding may cause permanent neurological deficits
- Seizures: Chronic irritation of brain tissue by AVMs can provoke epilepsy
- Learning and behavior problems: Especially in children with AVMs affecting critical brain regions
- Hydrocephalus: AVMs may obstruct the flow of cerebrospinal fluid, potentially causing fluid accumulation in the brain
- Pregnancy-related risks: Hormonal changes and elevated blood pressure during pregnancy may increase the risk of hemorrhage in people with AVMs
Untreated, AVMs can lead to progressive neurological decline or life-threatening emergencies. Early identification and, where appropriate, intervention are essential for minimizing irreversible injury.
Types of Central Nervous System Vascular Malformations
AVMs are the most recognized, but several vascular malformation subtypes exist within the central nervous system, each presenting unique challenges and risks:
| Type | Characteristics | Risks/Complications |
|---|---|---|
| Arteriovenous malformations (AVMs) | Abnormal tangles of arteries and veins, most commonly in brain or spinal cord | High risk of bleeding, seizures, stroke, neurological decline |
| Capillary telangiectasias | Widened, dilated capillaries often identified only via imaging | Typically benign; rarely cause symptoms or complications |
| Cavernous malformations | Clusters of misshapen, enlarged blood vessels appearing as mulberry-like lesions | Risk of seizures, hemorrhage, or neurological deficits if bleeding occurs |
| Dural arteriovenous fistulas | Abnormal connections between arteries and veins within the dura covering brain/spine | Risk of brain or spinal cord bleeding, neurological symptoms |
| Venous malformations | Enlarged veins in the CNS, often benign | Generally low risk, but complications possible if associated with other defects |
Arteriovenous Malformation in the Brain: Key Points
Brain AVMs can occur without symptoms for many years but can also lead to:
- Sudden, severe headache or neurological deficit (from bleeding)
- Seizure activity
- Chronic headaches or vision, speech, or coordination problems
- Increased risk of recurring bleeds if initial hemorrhage occurs
Early diagnosis and advanced treatment options have significantly improved the outlook for people with AVMs in recent years. Treatment may include microneurosurgery, endovascular embolization, or radiosurgery, depending on lesion size and location.
Arteriovenous Malformation in the Spinal Cord: Key Points
Spinal AVMs, while rare, may cause symptoms such as:
- Progressive weakness, numbness, or paralysis in the legs
- Sudden onset of back pain
- Loss of control over bladder and bowels
- Numbness or tingling sensations
- Headache or stiff neck in severe bleeds
Without timely intervention, spinal AVMs can cause lasting spinal cord damage. Early treatment, often surgical, is vital to prevent irreversible deficits.
Frequently Asked Questions (FAQs)
Q: Are arteriovenous malformations hereditary?
A: Most AVMs are not inherited, but some are seen in people with genetic conditions such as hereditary hemorrhagic telangiectasia (HHT), which increases the risk of abnormal vessel formation in the brain and other organs.
Q: What triggers an AVM to bleed?
A: AVM rupture often results from the increased pressure of arterial blood flowing directly into veins, which are not structured to handle such pressure. Any rise in blood pressure, trauma, or sometimes pregnancy can increase bleeding risk, but most bleeds occur unpredictably.
Q: Can an AVM heal on its own or go away?
A: AVMs generally do not resolve without treatment. Some small, incidentally found AVMs may remain stable for years, but active management is recommended if risk of bleeding or symptom progression is high. Treatment options include surgery, embolization, and radiosurgery.
Q: Who is at risk for developing an AVM?
A: AVMs can occur in anyone but are most often congenital. Having a genetic vascular condition (like HHT) or a family history of vascular malformations slightly increases risk. Most cases occur without clear cause or identifiable risk factor.
Q: How is an AVM diagnosed?
A: Diagnosis often involves imaging such as MRI, CT scan, or cerebral angiography. These tests detect abnormal vessel tangles or associated bleeding. AVMs may also be found incidentally when imaging is done for other reasons.
Key Takeaways
- AVMs are abnormal blood vessel tangles that can disrupt oxygen flow or bleed, causing neurological symptoms.
- Symptoms may be subtle or severe, varying by AVM location.
- Most AVMs are present at birth, with rare genetic associations.
- Major complications include hemorrhage, stroke, and neurological decline.
- Prompt diagnosis and specialized care improve outcomes.
Consult a medical specialist promptly if you experience neurological symptoms suggestive of an AVM.
References
- https://www.mayoclinic.org/diseases-conditions/brain-avm/symptoms-causes/syc-20350260
- https://www.mayoclinic.org/diseases-conditions/spinal-arteriovenous-malformation/symptoms-causes/syc-20355613
- https://www.mayoclinic.org/diseases-conditions/arteriovenous-malformation/diagnosis-treatment/drc-20454895
- https://medprofvideos.mayoclinic.org/videos/arteriovenous-malformations-avms-treatment-considerations-and-options
- https://www.mayoclinic.org/diseases-conditions/brain-avm/multimedia/brain-avm-video/vid-20426564
- https://www.youtube.com/watch?v=2s-J4TtKoEY
- https://www.mayoclinic.org/diseases-conditions/central-nervous-system-vascular-malformations/symptoms-causes/syc-20356113
Read full bio of Sneha Tete