A Comprehensive Guide to Hip Bursitis: Causes, Symptoms, and Effective Treatments
Discover everything you need to know about hip bursitis, from causes and symptoms to proven treatment options for lasting relief.
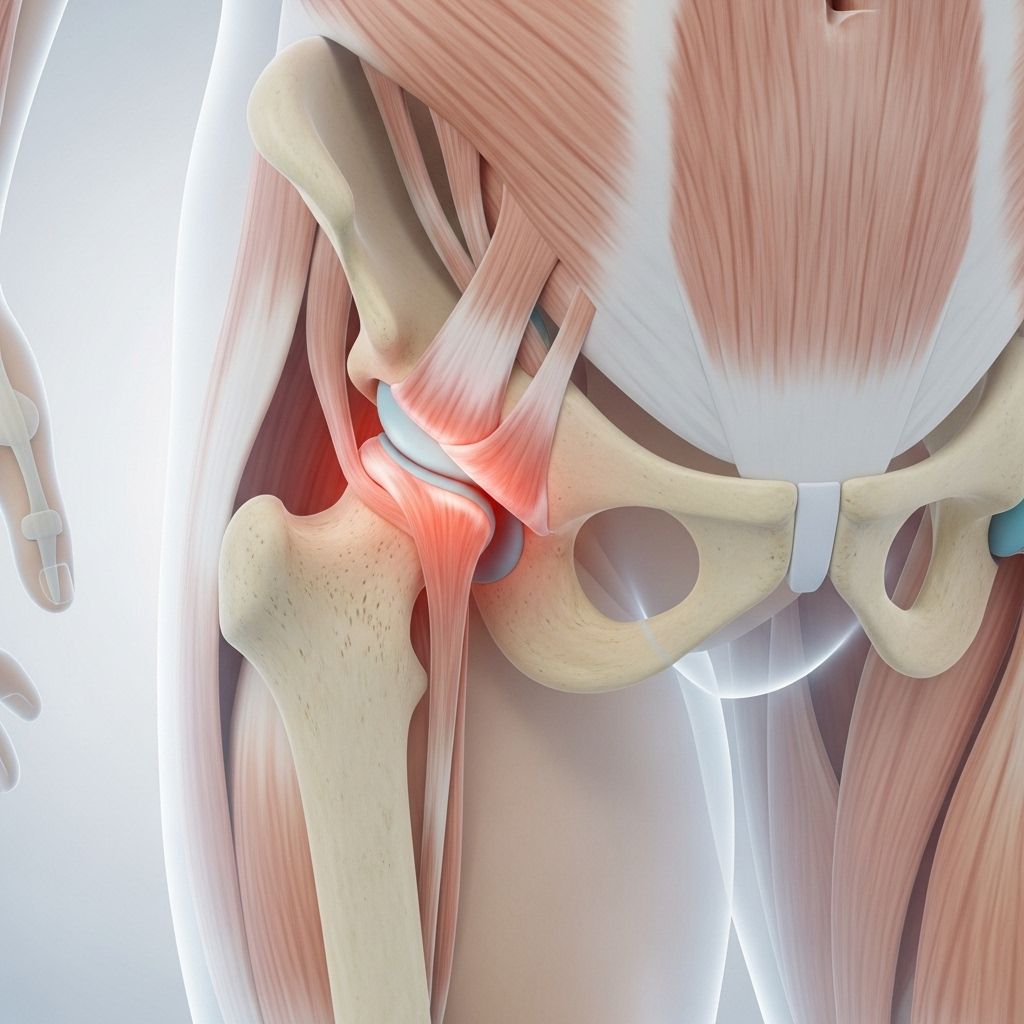
Understanding Hip Bursitis
Hip bursitis is a common orthopedic condition characterized by the inflammation of bursae—small fluid-filled sacs that reduce friction and cushion pressure points near your joints. These sacs protect tendons and muscles from rubbing against bone, but when they become inflamed, they can cause significant pain, discomfort, and restricted mobility. Among the numerous bursae in the human body, those around the hip—particularly the trochanteric bursa—are highly susceptible to bursitis.
This guide will walk you through the causes, symptoms, risk factors, diagnosis methods, prevention strategies, and best treatment options for hip bursitis, empowering you to recognize, manage, and prevent this condition effectively.
Types of Hip Bursitis
Hip bursitis can occur in any of the bursae located in and around the hip joint. The condition is classified depending on the location and cause of inflammation:
- Trochanteric bursitis: Inflammation of the bursa located over the greater trochanter (bony knob at the outside of your upper thigh), causing pain on the outside of the hip and outer thigh.
- Iliopsoas bursitis: Affects the bursa on the inside of the hip, leading to discomfort in the groin region.
- Ischial bursitis: Impacts the bursa near the upper buttocks area, less common but significant for certain pain patterns.
- Septic bursitis: In rare cases, the bursa may become infected, presenting serious symptoms requiring urgent medical attention.
Common Symptoms of Hip Bursitis
The symptoms of hip bursitis can develop gradually or appear suddenly after injury or overuse. Typical signs include:
- Pain around the hip or outer thigh, often sharp or aching
- Tenderness to the touch
- Swelling or visible warmth in the affected area
- Stiffness, especially after periods of inactivity or sleep
- Worsening pain during activities such as walking, climbing stairs, or lying on the affected side
- In septic bursitis: fever, fatigue, and redness around the hip area
Key Causes of Hip Bursitis
| Cause | Description |
|---|---|
| Repetitive Motions & Stress | Common in athletes and those with jobs/hobbies like carpet laying, gardening, or painting. |
| Acute Injury & Trauma | A direct blow, fall, or sudden overuse of the hip joint. |
| Inflammatory Arthritis | Conditions such as rheumatoid arthritis, gout, or pseudogout cause chronic joint inflammation. |
| Bacterial Infection | Occasionally, the bursa becomes infected (septic bursitis), leading to additional systemic symptoms. |
| Other Medical Conditions | Diabetes, spinal abnormalities (e.g., scoliosis), uneven leg lengths, and bony growths (bone spurs). |
Risk Factors
Although anyone can develop hip bursitis, certain factors and conditions increase your risk:
- Age: The likelihood increases with age.
- Repetitive activity: Jobs or hobbies involving repetitive motions or prolonged pressure on the hip.
- Pre-existing joint disease: Rheumatoid arthritis, gout, diabetes, or systemic inflammatory conditions.
- Obesity: Excess weight increases hip and knee stress.
- Structural abnormalities: Conditions such as scoliosis or unequal leg lengths affect gait and place additional stress on hip bursae.
How Hip Bursitis Is Diagnosed
Accurate diagnosis is essential, especially as hip bursitis shares symptoms with other joint conditions. Your healthcare provider will use a combination of history-taking, physical examination, and diagnostic imaging:
- Physical exam: Assessment of pain points, range of motion, and tenderness.
- Patient history: Consideration of risk factors, occupation, and recent activity changes.
- X-rays: Rules out underlying bone or joint disease.
- MRI scans: Provides detailed images of soft tissues, confirms inflammation of the bursa.
- Lab tests: For suspected infection (septic bursitis), tests may include blood counts and fluid analysis from the bursa.
Prevention and Lifestyle Management
Not all cases of hip bursitis can be prevented, but several lifestyle modifications can reduce the risk and severity of flare-ups:
- Use padding: Kneeling pads or cushions reduce hip pressure during repetitive activities.
- Lifting techniques: Bend your knees and keep heavy loads close to your body.
- Maintain a healthy weight: Reduces pressure on the hip and knee joints.
- Exercise regularly: Strengthening hip, back, and core muscles can greatly reduce bursitis risk.
- Warm up and stretch: Before strenuous activities, to protect joints from injury.
- Take regular breaks: Alternate repetitive tasks with rest periods.
- Posture correction: Good posture and ergonomics help prevent undue stress on joints.
Conservative Treatment Options
Most cases of hip bursitis respond well to non-surgical and home-based therapies, particularly if addressed early:
- RICE Therapy: Rest, Ice, Compression, and Elevation are critical in the initial management. Ice should be applied for 15-20 minutes several times a day to reduce swelling.
- NSAIDs: Nonsteroidal anti-inflammatory drugs (e.g., ibuprofen, naproxen) provide pain relief and reduce inflammation.
- Physical Therapy: Guided exercise routines aimed at stretching and strengthening hip muscles, improving posture, and correcting gait abnormalities.
- Assistive Devices: Temporary use of canes or crutches may relieve pressure during recovery.
- Moist Heat: After the first few days, heat therapy can ease stiffness and promote blood circulation.
Advanced Treatment Measures
When conservative treatments aren’t enough, healthcare providers may recommend more targeted interventions:
- Corticosteroid Injections: Direct injections into the bursa provide rapid symptom relief, especially for persistent or severe pain. These injections are generally safe but should be limited in frequency to prevent tissue damage.
- Antibiotics: For septic bursitis, a course of appropriate antibiotics is essential.
- Surgery: Rarely required, surgical removal of the bursa (bursectomy), or newer endoscopic techniques, can be performed for chronic cases unresponsive to other treatments. Both procedures are typically outpatient and do not disrupt normal hip function.
Recovery and Outlook
With early recognition and proper management, most people with hip bursitis recover fully and resume normal activity. Physical therapy, weight management, and modifications in daily activities contribute to long-term relief and help prevent recurrence. If left unmanaged or if the underlying causes are not addressed, flare-ups and chronic pain may develop.
Commonly Asked Questions About Hip Bursitis
Q: What is the difference between trochanteric bursitis and other forms of hip bursitis?
A: Trochanteric bursitis specifically affects the bursa over the greater trochanter, causing pain on the outer hip, while other forms impact bursae in the groin (iliopsoas) or upper buttock (ischial) regions.
Q: How long does it take to recover from hip bursitis?
A: Most cases improve within a few weeks with rest and treatment. Chronic bursitis or cases caused by underlying conditions may require longer recovery and physical therapy.
Q: Can I exercise while I have hip bursitis?
A: It is best to avoid activities that cause pain but continue approved stretching and strengthening exercises to aid recovery. Consult with a physical therapist or healthcare provider for recommended routines.
Q: Is hip bursitis preventable?
A: You can reduce risk by limiting stress on the hip, practicing proper lifting techniques, managing weight, and maintaining muscle strength and flexibility.
Q: When should I see a doctor for hip pain?
A: If pain is severe, persists beyond a few days, is accompanied by swelling, fever, or redness, or impacts mobility, you should consult your healthcare provider for evaluation and diagnosis.
Q: Is surgery for hip bursitis common?
A: Surgery is rarely needed and usually reserved for those who do not respond to conservative measures or have chronic, disabling pain.
Key Takeaways for Managing Hip Bursitis
- Address symptoms early for best outcomes.
- Combine rest, ice, stretches, and posture correction for effective pain relief.
- Consult with orthopedic specialists if pain persists or worsens.
- Follow recommended physical therapy to prevent recurrence.
- Adopt lifestyle changes (weight management, safe lifting) for long-term hip health.
References
- This guide synthesizes information from reputable medical sources on hip bursitis, including orthopedic associations, clinical resources, and healthcare providers.
References
- https://www.aurorahealthcare.org/services/orthopedics/conditions/hip-bursitis
- https://www.mayoclinic.org/diseases-conditions/bursitis/symptoms-causes/syc-20353242
- https://orthoinfo.aaos.org/en/diseases–conditions/hip-bursitis/
- https://familydoctor.org/condition/bursitis-of-the-hip/
- https://www.hoagorthopedicinstitute.com/what-hurts-/hip/conditions/hip-bursitis/
- https://my.clevelandclinic.org/health/diseases/4964-trochanteric-bursitis
- https://www.mayoclinic.org/diseases-conditions/bursitis/diagnosis-treatment/drc-20353247
- https://www.froedtert.com/orthopaedics/hip-preservation/hip-bursitis
- https://www.nhs.uk/conditions/bursitis/
- https://arksurgicalhospital.com/symptoms-solutions-hip-bursitis/
Read full bio of medha deb












